Conditions for the growth of microorganisms
Each type of bacteria requires individual living conditions: a certain level of acidity, humidity, viscosity, osmotic properties. In laboratory conditions, in order to determine the causative agent of the disease, it is sown on certain media, taking into account the characteristics of respiration, nutrition and reproduction of microorganisms.
There are environments in which several different types of bacteria can multiply and grow. Such living conditions are called universal (Sabouraud's medium, thioglycolate). Others are for one strain only (for example, staphylococcus and streptococcus are plated on saline or blood agar).
Purpose and significance of diagnosis
Microorganisms that land on human mucous membranes and skin can be divided into the following groups:
- Normal microflora are those bacteria that are permanent, safe residents. Without them, the human body cannot function properly, since representatives of normal microflora are involved in the processes of digesting food, synthesizing vitamins and enzymes. An insufficient number of microorganisms leads to the development of dysbiosis or bacterial vaginosis.
- Opportunistic pathogens - these strains are safe for humans only if the immune system is strong. If their living conditions change, bacteria begin to actively grow and multiply, causing pathology or disease.
- Pathogenic (disease-causing) microorganisms - they do not live in a healthy body. When accidentally infected, they cause the development of the disease, even death.
Microflora testing and sensitivity to antibiotics play a major role in the process of identifying bacteria, their strain, and species. This method is important for diagnosing diseases of infectious origin and sexually transmitted diseases.
Preparation of the expert group
First of all, you need to decide who will conduct the research. Teamwork is one of the key principles of FMEA. Only this format ensures the quality and objectivity of the examination, and also creates space for non-standard ideas. As a rule, a team consists of 5-9 people. It includes:
- project Manager;
- process engineer who develops the technological process;
- design engineer;
- representative of production or quality control service;
- employee of the consumer relations department.
If necessary, qualified specialists from third parties may be involved to analyze structures and processes. Discussion of possible problems and ways to solve them takes place in a series of meetings lasting up to 1.5 hours. They can be carried out either in full or in part (if the presence of certain experts is not necessary to resolve current issues).
Indications for testing
Microflora culture is not carried out as an independent analysis. It is prescribed by a doctor in cases where there is a suspicion that a pathogenic pathogen has entered the patient’s body or the growth and reproduction of opportunistic bacteria has been activated.
The following diagnostic measures are carried out:
- urogenital bacterial culture;
- bacterial culture from the nose, ear, pharynx, eye;
- bacterial culture of microflora from the wound;
- culture of urine, milk, bile, sperm, feces;
- bacterial culture for staphylococcus, mycoplasma, ureaplasma and other pathogens.
Carrying out the procedure
Taking a smear for bacteriological analysis is carried out in a laboratory:
- The patient sits on a couch or chair.
- To directly collect a swab from the oral cavity, the patient opens his mouth wide.
- The medical worker uses a special spatula to press the tongue to the lower jaw. Takes a microflora sample with a cotton swab.
- The swab is immediately placed in a sterile tube, which is tightly closed with a lid.
The procedure for taking a throat swab does not cause pain, but it can provoke a gag reflex. To minimize the process of reverse peristalsis, a person needs to properly prepare for the procedure - do not eat or drink anything.
See also
How to gargle with laryngitis for adults and children at home
Read
A sample of biological material is taken from the nose as follows: the patient sits on the couch and tilts his head back. The skin of the nostrils is disinfected with medical alcohol before the procedure. First, the laboratory assistant inserts a cotton swab into one nostril and rolls it over the surface of the mucous membranes. The procedure is then repeated with another sterile cotton swab from the next nostril.
In a child, the procedure for taking biological material is carried out according to the same algorithm as in an adult patient.
How to decipher the results
After receiving the results, I want to get acquainted with them immediately. The laboratory form states the following:
- Type of pathogen in Latin. Translating titles usually poses the greatest difficulty for curious readers. After reviewing the results, the doctor will tell you more about the type of pathogen and the characteristics of its reproduction.
- Quantitative indicators of microorganism growth. In most cases, colony-forming units of cells per 1 ml of material are used. For example, bacterial culture and sensitivity to antibiotics in urine with normal values should contain up to 103 CFU/ml. Results with high values may be questionable or indicate the presence of an inflammatory process.
- Clarification of the pathogenicity of the strain. This paragraph indicates whether the microorganism is pathogenic or opportunistic, living on the mucous membranes of the human body.
Indications
Microflora culture is widely used in medical practice in the diagnosis of infectious and inflammatory diseases (in gynecology, urology, venereology, otolaryngology, surgery and other areas), and at the risk of developing sepsis (a systemic reaction to developing inflammation). Antibiotic sensitivity testing allows us to identify and remove pathogens of the following diseases:
- bacterial vaginitis;
- infectious STDs (sexually transmitted diseases);
- chlamydia;
- gonorrhea;
- trichomoniasis;
- cystitis;
- intestinal infection;
- pneumonia;
- tuberculosis;
- sore throat and many others etc.
During pregnancy
Determination of sensitivity to antibiotics during pregnancy is carried out at least twice - immediately after registration and at 36 weeks. A smear is made from the vagina and the mucous membrane of the pharynx and nasopharynx. The biomaterial is examined to determine the presence of urological and genitourinary infections and Staphylococcus aureus, a pathogen that provokes purulent mastitis, postpartum sepsis and other infections in the period after delivery. If there are indications (kidney disease, increased levels of leukocytes in the urine, etc.), the following may be prescribed:
- urine culture;
- cervical smear;
- scraping of the vaginal epithelium;
- bacterial culture from the cervical canal.
Determination of pathogen sensitivity
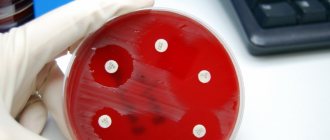
If the strain of a pathogenic microorganism is determined, it is inoculated in the laboratory on media with antibiotics. About those environments where growth will be the smallest or negative, specialists make notes on the result form. These antibacterial agents are considered the most effective when choosing treatment for the inflammatory process.
Since microflora culture is a fairly lengthy process (up to 7 days), drugs with a wide spectrum of action are first prescribed. Most microorganisms are resistant to one or another medication, which means a weekly dose may not only be ineffective, but also cost the patient a lot of money.
An antibioticogram, the decoding of which also requires the participation of a specialist, will allow you to choose the only effective remedy. The laboratory form indicates the following:
- strain and type of pathogen, its quantity in CFU/ml;
- names of antibacterial drugs indicating sensitivity (R, S, I) and zone.
Antibioticogram (decoding of Latin letters) says the following:
- R—pathogen resistant to the drug;
- I - the microorganism exhibits moderate resistance;
- S is a bacterium sensitive to this antibiotic.
Advantages of bacterial sowing
The method is highly specific - no cross-false reactions are observed. It is possible to examine any biological fluid. It is carried out in order to determine the sensitivity of the identified microbe to therapeutic agents, which allows the most effective therapy to be used.
The result is not obtained immediately. The requirements for material collection are high. Laboratory personnel must be highly qualified.
Indications for bacteriological culture
This method is widely used in medical practice, especially for infectious diseases, in gynecology, surgery, urology, oncology, otolaryngology, etc.
Absolute indications are any inflammatory diseases of organs and systems, suspicion of sepsis.
Material for research
The following materials can be examined: mucus from the throat, nasopharynx, cervical canal, urethra; sputum; feces; urine; blood; prostate secretion; breast milk; bile; cerebrospinal fluid; cyst contents; wound discharge.
What organisms are determined through bacteriological examination?
Mucus from the nose and throat may contain: hemolytic streptococci, pneumococci, Staphylococcus aureus, Corynobacter diphtheria, meningococcus, Haemophilus influenzae, listeria.
In stool you can find:
- intestinal group of bacteria - salmonella, shigella, yersinia;
- typhoparatyphoid group;
- opportunistic pathogens of intestinal infections;
- anaerobic microbes; foodborne pathogens;
- be examined for intestinal dysbiosis.
In the biopunctate, purulent discharge and wound contents, the following is isolated:
- pseudomonas;
- Pseudomonas aeruginosa.
Urogenital mucus is examined as follows:
- for the presence of pathogens of sexually transmitted infections - gonococcus, fungi, trichomonas, ureaplasma, listeria, mycoplasma;
- on bacterial flora.
Blood can be tested for sterility. Breast milk, prostate secretions, urine, smears, wound discharge, joint fluid, bile - these materials can be examined for contamination (bacterial flora).
Sowing the flora and its sensitivity to antibiotics: the research process
The collected material is placed in special media. Depending on the desired result, sowing is done in different media. For example, in a selective or elective medium, an example of which is coagulated horse serum to detect the causative agent of diphtheria, or a medium with bile salts/selenite to determine the causative agent of intestinal infections.
Another option is differential diagnostic media, which are used to decipher bacterial cultures.
If necessary, subculture from liquid to solid nutrient medium is done to identify colonies.
After this, the nutrient medium is placed in a thermostat, where favorable conditions are created for the life of pathogens. In this case, a specific time, humidity and temperature are set.
After removing the sample from the thermostat, a control examination of the grown microbial colonies (culture of microorganisms) is carried out. If necessary, microscopy of the resulting material with special staining is performed. Control examination - assessment of the shape, color, density of colonies.
Finally, the pathogens are counted. In laboratory practice, the concept of colony-forming unit (CFU) is used - one microbial cell that is capable of forming a colony, or a visible colony of microbes. The CFU indicator allows you to determine the number of microbes in a sample or determine their concentration. CFU counting can be done using different methods.
How to take an antibiotic sensitivity test
The quality of the test depends on several factors, including compliance with the rules when collecting material for research. Dishes and instruments must be sterile! Otherwise, contamination occurs (contamination with bacteria that have no clinical significance occurs), which makes the test meaningless.
If a person is taking antibiotics, cultures will not be accurate. These should be stopped 10 days before the expected date of analysis. You should also tell your doctor if you are taking any medications.
Delivery to the laboratory must be very fast; the material must not dry out or change its acidity.
For example, feces must be delivered warm.
- Urine collection is carried out after morning hygiene procedures. Collect an average portion of urine. The volume of urine is 10-15 ml. The utensils must be sterile. It must be delivered to the laboratory within 2 hours;
- If a nasal or throat swab is prescribed: do not brush your teeth, rinse your mouth/nose with disinfectants, eat or drink;
- Stool collection is carried out in the morning using a sterile spatula in the same container. Volume – 15-30 g. Urine is not allowed to get into it. Maximum delivery time is 5 hours. Freezing is not allowed. Feces are collected without laxatives or enemas;
- Blood is drawn before antibiotic therapy. The minimum amount is 5 ml for children, not less than 15 ml for adults;
- A sputum sample is taken in the morning on an empty stomach. Rinse your mouth and brush your teeth first. Delivered to the laboratory within a maximum of 1 hour;
- Breast milk is collected after water procedures. The skin around the nipple is treated with alcohol. Express 15 ml of milk, then squeeze the next 5 ml into a sterile container. It is delivered in 2 hours;
- Genital smear: collection is carried out at least 14 years after the end of menstruation, not earlier than a month after a course of antibiotics. Do not urinate for 2 hours for women and 5-6 hours before the test for men.
Intradermal test: determination of sensitivity to antibiotics
This test is carried out to determine whether a person is allergic to a specific medication. This allows, after identifying bacteria and determining their sensitivity to the antibiotic, to select treatment. But if a person has any contraindications to such medications, an intradermal test is performed to reduce the risk of adverse reactions.
The result of the study of mucus from the nasopharynx is ready after 5-7 days, bowel movements - 4-7, urogenital scraping - 7, culture for general flora - 4-7, blood for sterility - 10.
Explanation of antibiotic susceptibility testing
They take into account quality and quantity, that is, the very fact of the presence of microbes, as well as their concentration. Decoding the results is carried out using a very simple method.
In the material under study, several degrees of microorganism growth (contamination) are distinguished.
- First degree – no growth;
- second degree – growth on solid medium up to 10 colonies;
- third – up to 100;
- the fourth – more than 100 colonies.
The results are very important in identifying opportunistic microflora, since grades 1 and 2 are not considered to be the causes of the disease, but simply indicate contamination of the test material, but grades 3 and 4 indicate the cause of inflammation. When isolating pathogenic flora, absolutely all colonies are taken into account.
The results of counting CFU/ml are deciphered using the following method:
- 103/ml – one colony;
- 104/ml – from one to five;
- 105/ml – from 5;
- 106/ml – more than 15.
The number of colonies is important for determining the degree of pathology and monitoring therapy.
Antibiotic sensitivity: letters s and r in the analysis
An important component of diagnosis and treatment is determining the sensitivity of the pathogen to antibacterial drugs. The set of antibiotics to which the pathogen is resistant or sensitive is called an antibiogram. The sensitivity of a microorganism is when an antibiotic inhibits its reproduction. Resistance is the resistance of a bacterium, that is, the medicine will not affect it in any way. The antibioticogram is issued in specific units of measurement - the minimum inhibitory concentration (MIC).
As you can see, this issue can only be studied by a specialized specialist. I wish you health and good health!
Preparation for collecting material
Any biological fluids and smears taken from mucous membranes can serve as diagnostic material. More often, a smear for bacterial culture is prescribed by specialists in the field of urology and gynecology. To get the correct results, you need to properly prepare for collecting the material.
If the culture is performed on the patient's blood, then no special preparation is required. The only condition is to take the test on an empty stomach. The health worker takes venous blood, observing all the necessary rules of asepsis and antisepsis.
The conditions for donating urine are slightly different. In a healthy person, it is located in the bladder in the form of a sterile biological fluid. When urine passes through the female urethra, a small number of cocci can enter the material, which is taken into account during diagnosis and is considered normal (staphylococcus and streptococcus, diphtheroids). In men, the supply of urine with bacteria occurs in the anterior part of the urethra.
To reduce the possibility of other pathogenic microorganisms entering, the following rules should be followed:
- preliminary toilet of the genitals;
- use of a medium portion of urine;
- delivery to the laboratory within 2 hours after collecting the material;
- the test bottle must be sterilized or purchased from a pharmacy.
If material for bacterial culture is taken from the rectum, urethra, vagina, or cervical canal, then this occurs in private laboratories or medical institutions. Washing, douching and using antiseptics is prohibited, as this will distort the accuracy of the diagnosis.
How to get tested
Bacteriological culture for sensitivity to antibiotics is carried out on different types of biomaterial. Depending on their type, the following instructions from specialists must be observed when collecting samples:
- Urine collection is carried out in the morning, on an empty stomach, after preliminary hygiene procedures. The required volume of urine is from 10 to 15 ml. The collection is carried out in a special sterile container; the material must be delivered to the laboratory no later than two hours later.
- A swab test for sensitivity to antibiotics from the nasopharynx or throat is carried out in the morning, before eating and drinking water and before performing hygiene procedures (brushing your teeth and rinsing your mouth).
- Feces are collected in the morning, using a sterile spatula in a sterile container, the required volume of biomaterial is up to 30 mg. Avoid contact with urine, use of enemas or laxatives, or freezing. Delivery time to the laboratory should not exceed 3-5 hours.
- The sputum sample is delivered to the study site within an hour after collection, which is carried out on an empty stomach, after preliminary brushing of the teeth and rinsing the mouth.
- A breast milk sample is taken after hygiene procedures and treating the skin around the nipple with alcohol. Before collecting material in a volume of 5 ml (in a sterile container), 15 ml of liquid is decanted. Delivery time to the laboratory should not exceed 2 hours.
- A smear from the vaginal mucosa and other types of sampling for genitourinary infections. The analysis is carried out no earlier than 2 weeks after the end of menstruation (the exact date will be determined by the doctor based on data on the monthly cycle). The last urination should be carried out two hours before taking the sample in women and 5-6 in men.
- The volume of blood collected for culture in children is 5 ml, in adults – 15 ml.
Stool culture
The intestinal tract has permanent “residents” who participate in the processes of digestion, the synthesis of vitamins and enzymes. The ratio of bacteria is constant and may fluctuate slightly in one direction or another.
When immune forces are reduced, pathogens enter the body, or antibiotics are taken for a long time, the normal ratio is disrupted. The number of lactobacilli and bifidobacteria decreases sharply, and their place can be taken by pathogenic strains of Escherichia coli, Proteus, Clostridia, Pseudomonas aeruginosa, yeasts, etc.
Stool for diagnostic purposes is collected in a sterile transport container. The sowing result is ready in 3 to 7 days.
Crops during pregnancy
During pregnancy, culture is a mandatory diagnostic method and is carried out twice: during registration and at 36 weeks. A smear is taken from the genital tract, as well as the nose and throat. Thus, the presence of urogenital inflammatory processes and carriage of Staphylococcus aureus is determined. Pregnant women also donate urine to be cultured for sterility.
A nuisance that can be detected is E. coli in a smear in women. Treatment for this condition should be immediate. This is especially true for pregnant women, because the presence of pathogenic microflora can lead to infection of the baby during passage through the birth canal. If E. coli is detected in a smear in women, treatment is prescribed by a gynecologist. A combination of local therapy and systemic drugs is used.
The objects of search during the period of bearing a child are chlamydia, fungi, mycoplasma, ureaplasma, and trichomonas.
To whom and when is the test prescribed?
Urinary tract infections occupy a significant place in the structure of morbidity, among them are urethritis, cystitis, and pyelonephritis.
Often these patients are prescribed a urine test to identify the causative agent of the disease and correct treatment.
Another purpose of the study is to monitor urine contamination after long-term catheterization of the bladder, as well as to monitor treatment.
It is advisable to take a urine test before starting antimicrobial therapy or during the break between courses. It is better if 5-7 days have passed after finishing the antibiotic course. The referral must indicate the use of antibiotics, its type and course.
Also, a urine flora test is indicated for all patients upon hospitalization in an infectious diseases hospital (regardless of the diagnosis).
For screening purposes, all pregnant women undergo urine culture twice during pregnancy:
- when registering;
- at 36 weeks.
Such control for the presence of pathogenic flora can significantly reduce the frequency of cystitis and pyelonephritis in pregnant women.
Gynecologist - online consultations
Help decipher the analysis: Sowing for flora and sensitivity
Hello! Help decipher the analysis: Culture of flora with determination of sensitivity to antibiotics. Isolated flora Escherichia coli Quantity: abundant growth (10^6 and above) Norm: less than 1×10^4 Pathogenicity: Opportunistic flora Sensitivity to antibiotics Species m/o Escherichia coli Amikacin 20mm (S) Sensitive Ampicillin 18mm (S) Sensitive Co-trimoxazole 2mm (R) Resistant Levomycetin 24mm (S) Sensitive Ceftriaxone 2mm (R) Resistant Ciprofloxacin 24mm (S) Sensitive
Milovskaya Olga, St. Petersburg
Hello Olga! Where (S) Sensitive - the microorganism dies under the influence of the antibiotic, where (R) Resistant - the antibiotic does not affect the microorganism and, accordingly, there is no point in treating with this antibiotic. Best wishes!
Hello, I took a flora test to determine sensitivity to antibiotics, the method was microbiological. Help me decipher. Ultrasound is normal. Isolated flora - Escherichis coli, quantity - abundant growth (10^6 and above), norm - less than 1^10^4, pathogenicity - conditionally pathogenic flora. Antibiotic sensitivity: Amikacin -10 mm - resistant, Meropenem - 26 mm - sensitive, Ceftriaxone - 27 mm - sensitive, Ciprofloxacin - 27 mm - sensitive. Thank you!
Hello, please help me decipher my husband’s analysis. Flat epithelium (in the visual field) - 4-5 Transitional epithelium (in the visual field) -10-15 Leukocytes (in the visual field) -0-5, up to 10 Erythrocytes -0 Gram (+) cocci -1 Gram (- )cocci- — Gram+-coccobacillary flora -2 Mucus-2 There is nothing else, everything is negative. There are no hidden ones either. My E. coli was -10 to the fifth power. And a frozen pregnancy. Now we are looking for reasons. Does he have this E. coli? Should he treat her? Help me please! And further.
Pregnancy 27-28 weeks. A month ago, stitches were placed on the cervix (at 21 weeks. The reason was that the cervix was amputated a year ago). A week before suturing, a course of antibacterial therapy was completed (amoxiclav intravenously for 7 days), which was carried out due to the identified infection with Enterococcus fecalis. Now the culture again shows the active growth of fecal matter and E. coli, there are no leukocytes in the smear yet, the sutures are clean. There is sensitivity to a wide range of antibiotics, but clinical pharmacologist Dr.
Culture of flora with determination of sensitivity to antibiotics Isolated flora: Staphylococcus epidermidis Quantity: meager growth (10^2-10^3) Norm: less than 1x10^5 Pathogenicity: normal flora
Cytological follow-up of a mixed scraping of the cervix and cervical canal The quality of the preparation is adequate Cytogram (description) The cytogram corresponds to the inflammatory process of the mucous membrane with a reactive change in the epithelium. Please tell me what this means and why it is dangerous.
Dear doctor! I am writing to you with the following question: My name is Christina, my husband and I are planning a pregnancy; I have been diagnosed with Ureaplasma spp. 10^6 I completed a full course of treatment with antibiotics (Vilprofen, Flemoclav Solutab, Polygynax), my husband had a tank done. Sowing on ureaplasma species with determination of titer and sensitivity to antibiotics, the result of the analysis showed meager growth (less than 10^4) without antibiotic parameters, since we were told that it was not possible to detect sensitivity to antibiotics in this way.
18+ Online consultations are for informational purposes only and do not replace a face-to-face consultation with a doctor. Terms of use
Your personal data is securely protected. Payments and site operation are carried out using the secure SSL protocol.
How long does it take to sow?
Cultures for flora and sensitivity to antibiotics are carried out for some long time (compared to the readiness of the results of other tests). Isolation of strains is not carried out in the same way, because different biological environments of the human body require individual approaches. Approximate timing of test results for different types of biomaterial:
- Feces: from 5 days to a week.
- Urogenital materials: 4-10 days.
- Blood: 10-14 days (the first preliminary data are ready in 3-4 days).
- Mucus from the throat or nasopharynx: from 5 to 7 days.
- Sowing on flora: 5-10 days.
- The most effective diets for losing weight at home: menus and reviews
- How to get rid of calluses on your toes
- The sofa cover is universal and has an elastic band. How to sew a cover for a sofa and armchairs with your own hands
Analysis of sputum for microflora and sensitivity to antibiotics
general description
It is a microbiological study of discharge from the lower respiratory tract to determine the type of microorganism and select adequate therapy. Main indications for use: inflammatory diseases of the respiratory tract (pneumonia, acute and chronic bronchitis, lung abscess). Typically, sputum is obtained by coughing or tracheal aspiration.
Pathogens of lower respiratory tract infections are divided into three groups according to the degree of pathogenicity:
- Pathogens of high priority are Staphylococcus aureus, Haemophilus influensae, Klebsiella pneumoniae, Streptococcus pneumoniae.
- Medium level - Candida albicans, Moraxella (Branhamella) cataralis, enterobacteria.
- Low pathogenic - Mycoplasma pneumonia, Pseudomonas aeruginosa, Chlamydia spp. Legionella pneumophila and a number of other microorganisms.
When interpreting the data obtained, it should be taken into account that in persons with reduced immunity, representatives of the normal flora in quantitative terms can significantly exceed their normal values, and in this case this flora is considered as the causative agent of infection. For sputum, a clinically significant number is considered to be 106-107 CFU/ml. For bronchial washings after bronchoalveolar lavage - 104-105 CFU/ml.
The numerical values of the contamination units are interpreted as follows: for example, bacteria 102 were detected, this means that 100 colony-forming units of bacteria were detected in 1 ml of biological material, since the degree number (in this example it is the number 2) indicates the degree of contamination. If 103, then 1000 colony-forming units of bacteria in 1 ml of biological material.
Due to the fact that sputum usually contains oropharyngeal microflora, the culture result should be interpreted taking into account the clinical picture and general condition of the patient.
Bacteria leading to the development of respiratory tract pathology include Staphylococcus aureus, Haemophilus influenzae, Pseudomonas aeruginosa, Streptococcus pyogenes, Streptococcus pneumoniae, Moraxella catarrhalis, fungi of the genus Candida, Nocardia asteroides and N. cavia, Acinetobacter baumannii, Chlamydia psittaci and Mycobacterium tuberculosis - 100 %.
Norms
Normally, human sputum is contaminated (contaminated) with the following types of normal symbiotic microflora characteristic of the upper respiratory tract: Staphylococcus spp. Streptococcus viridans group. Corynebacterium spp. (except Corynebacterium diphtheria), Neisseria spp. (except Neisseria meningitidis), Bacteroides spp. Veillonella spp. Lactobacillus spp. Candida spp. Diphtheroids, Fusobacterium spp.
Diseases for which the doctor may prescribe a sputum test for microflora and sensitivity to antibiotics
Description of the analysis
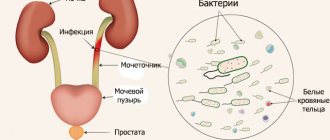
Urine culture is a microbiological examination of urine, which is prescribed to check the genitourinary tract for infection. The purpose of diagnostics is to identify pathogenic microorganisms and select medications necessary to normalize a person’s condition.
During the analysis, special attention is paid to the types of microbes found and their concentration in relation to the entire volume of urine. An antibiogram can also be performed - checking the susceptibility of microorganisms to medications. If any infectious agent is detected in the urine, bacteriuria is diagnosed.
What bacteria does it detect?
A urine microflora test should be prescribed twice, including an initial study to identify the causative agent of the infection, as well as a control diagnosis. Through this study, the following can be detected in the patient’s urine:
- streptococci;
- staphylococci;
- enterococci;
- candida;
- Proteus;
- Escherichia;
- Klebsiella
It is important to know! Normally, no type of bacteria should be detected in the urine of a healthy person. But since microorganisms from the environment could have entered the analysis, their minimum content in urine still becomes possible. Therefore, to check the objectivity of the results obtained, specialists order a repeat study.
In what cases is it prescribed
Before the examination, the doctor collects a medical history (in other words, the patient’s complaints), and only then, based on the data obtained, makes preliminary conclusions. A urine flora analysis must be prescribed to a patient if the following symptoms occur:
- discomfort in the lumbar region;
- pain in the perineum;
- pain and burning during urination;
- the appearance of blood or pus in the urine;
- change in urine color;
- severe swelling of the limbs and face;
- low-grade fever for several days;
- regular headaches;
- general weakness.
Some pathological conditions may also be the reason for taking a bacteriological examination of urine:
- kidney tuberculosis;
- diabetes;
- systemic and local infections;
- urolithiasis disease;
- neoplasms in the genitourinary system;
- HIV.
Additionally, urine culture is needed to monitor the degree of effectiveness of the prescribed treatment and monitor the health of a person with immunodeficiency disorders. It is also recommended to take the test during pregnancy.
Sowing on flora
general description
This is a microbiological study that makes it possible to determine the qualitative and quantitative composition of the microflora of the biomaterial under study, including the identification of high-titer opportunistic microorganisms and pathogenic microorganisms, and their sensitivity to antibiotics.
Method capabilities
- accurate identification of the causative agent of infectious diseases;
- development of rational antimicrobial therapy in each specific case;
- assessment of the degree of effectiveness of the therapy.
Indications for the study
- inflammatory diseases of any location except the intestines.
Material for research
- a single portion of urine,
- urogenital smear (with prostate secretion),
- sputum,
- oropharyngeal swab,
- nasopharyngeal swab,
- breast milk,
- ejaculate,
- discharge from the ear,
- conjunctival smear,
- synovial fluid,
- cerebrospinal fluid,
- smear from the cervical canal,
- urethral smear,
- pleural fluid,
- flushing from the bronchi,
- bile,
- exudate,
- biopsies.
Preparing for the study
- the patient drinks a large amount of water at least 8-12 hours before collecting sputum;
- urine culture for flora should be carried out provided that diuretics are excluded within 48 hours before urine collection;
- For women, urine or urogenital smear testing is performed before the onset of menstruation or 2 days after its end;
- for men, it is recommended not to urinate for at least 3 hours before giving urine or a smear;
- On the day of taking biomaterial for analysis, patients are prohibited from brushing their teeth.
Interpretation of research results
Normal human microflora is a collection of microorganisms that inhabit the skin and mucous membranes. The largest number of them live in the gastrointestinal tract, the rest - on the skin, pharynx, pharynx, and genitourinary system. Normal microflora is divided into permanent, facultative and random. Reference values for various types of microorganisms depend on their location (point of collection of biological material). Thus, biological material obtained from the pharynx and nose is used to determine the nature of the nonspecific infectious process occurring in the body. Also, scraping from the nose is relevant when testing for sensitivity to antibiotics.
Based on their ability to cause infectious diseases, microorganisms are classified into non-pathogenic (not causing disease), opportunistic (normally they can be released in small quantities and, under certain conditions, actively multiply, leading to inflammation) and pathogenic (they are causative agents of infectious diseases and are not part of the normal microflora). are detected).
When opportunistic microorganisms are detected in high titers or pathogenic microorganisms, their sensitivity to antibiotics and bacteriophages is determined.
In both men and women, the results of the study may be influenced by previous antifungal or antibacterial therapy.
Norms
The norm is the presence in the microflora of non-pathogenic microorganisms, opportunistic microorganisms in small quantities and the absence of pathogenic ones.
Sources: No comments yet!
Sowing on flora with determination of sensitivity to antibiotics is an accurate microbiological analysis that takes place in the laboratory. For research, biological material is taken and placed in an environment favorable for the development of pathogenic microorganisms.
It allows the doctor to make a correct diagnosis and immediately determine the group of effective antibiotics.
Indications for the procedure
A smear is taken to study the composition of the microflora of the nasopharynx, to identify the causative agent of the pathology, and its sensitivity to antibiotics.
In what cases is a smear prescribed:
- prolonged runny nose that does not go away for more than 7 days;
- allergy;
- frequent relapses of pharyngitis, tonsillitis, laryngitis;
- diagnosis of streptococcal sore throat;
- the presence of manifestations of infections caused by Staphylococcus aureus;
- if you suspect diphtheria, whooping cough, meningitis, fungal pathologies;
- tuberculosis;
- sinusitis, adenoiditis;
- mononucleosis, abscesses.
A throat swab is part of a preventive examination; the test is prescribed for children attending educational institutions, health workers, people who work with food or in preschool and school institutions.
A smear to determine the composition of the microflora of the ENT organs is prescribed to all pregnant women.
Compliance with the rules of preparation for taking a smear largely determines the reliability of the results.
Preparation rules:
- stop taking antibacterial drugs in the form of tablets for a week;
- 5 days in advance, stop using sprays, ointments, rinses with antibacterial and antiseptic effects;
- Before collecting material from the oropharynx, you should not eat, drink, chew gum, or smoke; if it is necessary to do an oral cavity analysis, it is contraindicated to brush your teeth.
Stop taking antibiotics a week before your test.
The reliability of the analysis is also affected by the professionalism of the medical personnel; if there are errors during the collection, storage and transportation of the biomaterial, the culture result will be unreliable.
Procedure technique:
- The patient opens his mouth wide and throws his head back.
- The nurse presses on the tongue with a sterile or disposable spatula and collects mucus and plaque from the mucous membranes of the pharynx and tonsil surfaces with a cotton swab.
- The resulting material is placed in a test tube with a nutrient solution, which allows the bacteria to remain viable during transportation.
- The resulting biomaterial is sent to the laboratory, delivery time is no more than 2 hours.
Taking a smear is a painless but unpleasant procedure; pressing on the tongue can provoke an attack of vomiting, especially if the material is taken from a child.
Before examining the nasal mucosa, mucus is removed, crusts are removed, and the skin of the nostrils is lubricated with medical alcohol. The patient tilts his head back a little, and a sterile swab is passed alternately along the walls of the right and left nasal passages. The samples collected in a test tube are sent to the laboratory.
During microscopic examination, the resulting biomaterial is Gram stained and examined after treatment with immersion oils. The method allows you to identify gram-positive and gram-negative bacteria, coccal flora, and coccobacilli.
Bacteriological culture is one of the main diagnostic methods, since each microorganism can multiply only in a certain environment, at a comfortable level of pH and humidity; during the study it is important to maintain complete sterility.
Bacteriological culture is the main type of diagnostics for identifying pathogenic microorganisms
If an increase in microflora is detected, antibiotic sensitivity tests must be carried out; many microbes are able to quickly develop immunity to drugs - in the presence of ineffective therapy, severe complications develop.
A fingerprint smear is a specific analysis for studying the composition of cells in the nasal mucosa. The sample is applied to a glass slide, and the number of eosinophils and other particles is counted. The study is prescribed if you are predisposed to allergies.
If antibacterial therapy is ineffective, phage sensitivity tests are performed. The result allows us to select bacteriophages to eliminate the manifestations of infectious pathologies - these are modern antimicrobial drugs that cause the death of only certain types of bacteria.
About 50 beneficial microbes, representatives of saprophytic and opportunistic microflora live on the mucous membranes of each person; the study of discharge from the throat and nose makes it possible to determine the quantitative ratio and composition of etiologically significant microorganisms.
List of microbes
| Safe microorganisms: | Dangerous microorganisms |
|
|
The result is entered into the form, indicating the genus, type, number of microorganisms, and level of pathogenicity. After determining the type of pathogen, tests are carried out to determine the sensitivity of microbes to antibacterial agents and bacteriophages.
A negative result indicates the absence of fungi and pathogenic bacteria, which means that the infection is of viral origin. A positive result is observed in the presence of dangerous microorganisms, or the active growth of representatives of opportunistic microflora.
In terms of time, a bacteriological examination takes 5–7 days; in emergency cases, a rapid test is done to identify antigens to bacteria and fungi; the result can be obtained within half an hour.
The presence of a large number of fungi and bacteria in a smear is a sign of the development of ENT diseases; each microorganism provokes certain pathologies.
Exceeding the norm of staphylococci is most often observed in children
What diseases are caused by pathogenic microorganisms:
- staphylococci - pharyngitis, tonsillitis, gingivitis, sinusitis, active growth of bacteria is most often observed in children and the elderly;
- streptococci - sore throat, scarlet fever, sinusitis;
- fungi of the genus Candida - oral candidiasis, often accompanied by complications that affect the organs of the respiratory system;
- pneumococci, neisseria - pneumonia, bronchitis, otitis media, osteomyelitis, diseases of the upper respiratory tract, oropharynx;
- diphtheria pertussis, normally there are no bacteria in the smear; if the result is positive, the concentration level of microbes is determined to make a conclusion about the degree of development of the pathology;
- hemolytic streptococcus - severe forms of sore throat, which almost always cause heart complications.
With indicators of more than 10*5–10*7 CFU/ml, the likelihood of developing inflammatory, infectious, purulent processes is maximum. The draining result is a very high content of pathogenic microbes, their number cannot be counted, it is observed in severe and advanced forms of the disease, and urgent antibacterial therapy is required.
A nasopharyngeal smear is an effective method for diagnosing diseases of the ENT organs, determines the type of causative agent of the pathological process, the stage of development of the disease, allows you to select effective methods of therapy and reduce the risk of complications.
What organisms does it show?
Each type of biological fluid belongs to a specific system. And the systems, in turn, have sets of common diseases. After passing the test, a positive answer may indicate the presence of the following organisms.
Oral and nasal examinations:
- Staphylococcus aureus;
- Meningococcus;
- Haemophilus influenzae;
- Hemolytic streptococcus;
- Pneumococci;
Stool examination:
- Specific intestinal bacteria - salmonella, yersinia, shigella;
- Typhoparatyphoid bacteria;
- Conditionally pathogenic pathogens;
- Dysbacteriosis;
Study of problematic and purulent wounds:
- Pseudomonas;
- Pseudomonas aeruginosa;
Examination of the genital organs:
- Trichomonas;
- Gonococcus;
- Listeria;
- Ureaplasma;
- Bacterial flora;
Other types of research:
- Study of the general condition of the flora and detection of pathogens of inflammatory processes.
The bacterial culture method always makes an accurate diagnosis, but you need to understand how this or that biological fluid is collected so as not to personally influence the incorrectness of the result.
Types of microorganisms studied
Depending on the type of biomaterial and indications for analysis, the following types of pathogenic agents of bacterial infections are distinguished based on the results of the study:
- Mucus from the nasopharynx and pharynx: Staphylococcus aureus, hemolytic streptococcus, meningococcus, listeria, Corynebacterium diphtheria, Haemophilus influenzae, Pseudomonas aeruginosa.
- Purulent discharge, wound contents, biopunctate: Pseudomonas aeruginosa, pseudomonas.
- Urogenital mucus: bacterial flora, pathogens of genitourinary infections (mycoplasma, gardnerella, ureaplasma, trichomonas, fungi, gonococcus, listeria).
- Feces: typhoparatyphoid bacterial group, intestinal group (Yersinia, Salmonella, Shigella), anaerobic pathogens of food infections, opportunistic pathogens of intestinal infections.
- The blood is examined for sterility.
- The rest of the biological fluids are tested for contamination (bacterial flora).
Research process
Taking into account the localization of inflammation and symptoms, specialists place the collected material in a certain environment.
For example, a medium with bile salts indicates an intestinal infection, an elective medium identifies the causative agent of diphtheria, and differential diagnostic media can indicate a specific bacteriological culture.
The second stage of the study is the cultivation of colonies of microbes that have been discovered. To do this, they are placed in a thermostat, where all parameters are adjusted for favorable development.
The third stage is counting the number of pathogens. These can be individual bacteria or entire colonies. Sometimes colonies are examined under a microscope to determine treatment.
Material for bacterial inoculation: basic rules
Despite the professional work of the laboratory, much depends on the patient himself. If he does not adhere to the rules for collecting material, then the research will be considered invalid.
Please pay attention to several important aspects:
- Sterility! This applies to both containers and instruments used to collect biological fluid.
- Stop antibiotics for 10 days. Informing your doctor about all medications you are taking.
- Fast delivery to the laboratory. The material cannot be stored for more than a few hours, as its acidity changes.
In addition, each type of material has its own collection nuances. Urine is given in the morning after washing. Volume – 10-15 ml. It must be submitted within 2 hours. When you go to have your mouth or nose swabbed, you should not eat anything, drink anything, rinse your mouth, or brush your teeth.
A special sterile container is used to collect stool. Volume – 10-15 g. Deliver it within 5 hours. Under no circumstances should you use an enema or laxatives. It is forbidden to place feces in the refrigerator.
Sputum is collected in the morning on an empty stomach. Before doing this, you should brush your teeth. Must be submitted within 1 hour. Breast milk is collected only after a thorough shower. Nipples are treated with alcohol. Volume – 5 ml. The material must be delivered within 2 hours.
There are no rules for donating blood. But you need to remember about antibiotics. No medications for 10 days. And genital smears require no medications for a month. Women should not have a smear test during the first 2 weeks of their cycle.
Before the procedure, women should not urinate for 2 hours and men for 5 hours.
Reliability of results
The results of bacteriological examination of urine are highly reliable and informative if the rules for collecting and processing the material are followed.
The following factors influence the accuracy of the study results:
- sterility of the utensils used;
- compliance with urine collection rules;
- deadlines for submitting material for analysis;
- sufficient qualifications and accuracy of laboratory personnel.
The patient will have to be tested again if:
- the terms of collection were violated;
- tests were taken while taking medications;
- urine has an unusual color due to unauthorized food or menstruation.
Decoding
The result of the study has two main meanings:
- Firstly, this is the presence of a certain bacterium.
- Secondly, its concentration in the body. You don't have to be an expert to decipher the data received.
There are 4 degrees of growth of microorganisms in the body:
- The first and second degrees are not dangerous. They talk about the presence of up to 10 colonies of bacteria. But these readings do not indicate a diagnosis, but rather evidence of contamination of the material itself.
- The third (up to 100 colonies) and fourth (more than 100 colonies) degrees already indicate a problem. The number of colonies is an important indicator, since it is used to determine the degree of diagnosis.
Antibiotic sensitivity test
This test shows which antibiotics can cope with pathogenic bacteria. If the patient is allergic to a certain group of drugs, then the treatment will not have the desired effect.
The study shows how the collected material reacts to a particular antibiotic. This allows you to find the best solution and start professional treatment immediately.
Particular attention should be paid to the letters R and S. If you see the letter R in the results, it means that the bacteria are not susceptible to the action of the antibiotic, if S, then an excellent treatment method has been found.