You are here: Blood test -
Red blood cells -
Hypochromia of red blood cells
- Etiology
- Classification
- Symptoms
- Diagnostics
- Treatment
- Possible complications
- Prevention and prognosis
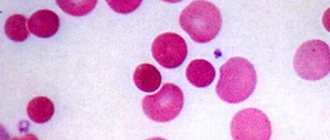
Hypochromia of erythrocytes (syn. hypochromic anemia) is a change in the saturation of red blood cells with hemoglobin, against the background of which their color changes (the cells become pale pink), and the central area becomes more extensive. Such a deviation can occur in every person, regardless of parameters such as age and gender.
Anisocytosis can be provoked by a large number of predisposing factors, which do not always have a pathological basis. This means that the problem can occur in a completely healthy person.
The symptoms of hypochromia are nonspecific; moreover, the ailment may go unnoticed, since the signs of the underlying disease come to the fore. The main manifestations are dizziness and pale skin, constant weakness and drowsiness, frequent mood swings.
The main diagnostic measure is a general clinical blood test. To search for a particular provocateur, additional laboratory and instrumental examinations are used.
Hypochromic red blood cells are eliminated using conservative methods of therapy, including folk remedies, following a gentle diet and taking oral medications. It is impossible to completely get rid of the problem without eliminating the original source.
Etiology
In a healthy body, the color value of red blood cells varies from 0.85 to 1.05. When acceptable indicators deviate from the norm to a lesser extent, it is advisable to talk about hypochromia. The problem is very often combined with disorders such as anisocytosis (change in cell size above or below acceptable values) or poikilocytosis (irregular shape of red blood cells).
Today, the main reasons for this deviation are:
- iron deficiency in the body;
- increased consumption of such a microelement;
- improper absorption of iron by the intestines.
As for predisposing factors, they are divided into 2 large categories - pathological and physiological. The first group of provocateurs:
- heavy blood loss;
- chronic bleeding, including nasal and uterine bleeding, hemorrhage from the gums and organs of the digestive system;
- Crohn's disease;
- enteritis;
- celiac disease;
- gastritis;
- helminthiasis;
- intestinal infections;
- irritable bowel syndrome;
- nonspecific ulcerative colitis;
- malignant blood diseases;
- oncological neoplasms - the most dangerous are those tumors whose focus is in the gastrointestinal tract;
- severe poisoning with chemicals and toxic substances;
- pyelonephritis;
- tuberculosis;
- infectious diseases in chronic form;
- pneumonia;
- any autoimmune processes.
Less harmless sources of the formation of hypochromic red blood cells:
- frequent donation - more than 4 times a year;
- previous surgical interventions;
- uncontrolled use of certain groups of medications;
- hormonal imbalance;
- the course of menstruation in women;
- period of bearing a child;
- breast-feeding;
- prolonged refusal to eat or adherence to excessively strict diets;
- poor nutrition;
- the effects of stress over a long period of time.
The main risk group includes people from 15 to 50 years old. Hypochromia of red blood cells is more often diagnosed in females than in males.
Degeneratively changed and normal red blood cells
Reasons for development
The normochromic type of anemia can be provoked by the following pathological processes:
- Hereditary diseases.
- Iron deficiency. A deficiency of the element can be caused by poor nutrition, blood loss, stomach ulcers or tumors in the small intestine.
- Age-related changes. The number of red blood cells drops sharply in women after 80 years of age.
- Infectious and inflammatory processes.
- Severe blood loss.
- Chronic form of renal failure.
- The presence of a malignant neoplasm or cancerous degeneration of cells. In this case, a macrocytic normochromic type of anemia develops.
In most cases, normochromic anemia develops in patients with kidney disease. When the functioning of the organs of the urinary system deteriorates, uremic toxins are released back into the blood, which is why the life of red blood cells is sharply reduced from 120 days to 40-60 days. Hemodialysis also has a negative effect. During the procedure, the body loses up to 1 g of iron annually, while the body of a healthy person contains only 4 g of the chemical element. In addition, with poor kidney function, the production of erythropoietin deteriorates.
Important information: How to treat iron deficiency anemia in young children (children) and symptoms of IDA
Classification
Hypochromia of erythrocytes can occur in several forms:
- iron deficiency anemia - considered the most common option and is characterized by an absolute decrease in iron;
- sideroblastic anemia - the content of the main microelement is within normal limits, but it does not participate in the synthesis of iron-containing protein;
- iron redistribution anemia - an excess of iron is detected, but this is accompanied by the breakdown of red blood cells;
- mixed anemia.
There are several degrees of severity of the problem, which are determined by the level of hemoglobin. Hypochromia happens:
- mild - the level of the main component of red blood cells is above 90 g/l;
- moderate - concentration varies from 70 to 90 g/l;
- heavy - parameters do not reach 70 g/l.
General blood test and laboratory practice
Modern clinical medicine has powerful research tools for studying the tissues of the human body, making it possible to accurately determine the amount of hemoglobin in the blood - a protein containing iron. Such capabilities eliminate the need to determine the iron content “by eye” by assessing its color range and other sensitive parameters. However, modern equipment is not available in all corners of our big world, which maintains the relevance of traditional research methods.
Blood color index
Hypochromia is an outdated but relevant term. Its use in current laboratory realities is a tribute to tradition. In those days when medical laboratories did not have the ability to conduct detailed biochemical studies of red blood cells, the main way to obtain information about the state of red blood cells was a microscope. The laboratory assistant visually examined the red blood cells, assessing their color, volume, shape, and size. The color of red blood cells served as a justification for the amount of iron in the body - if it was bright and saturated, then it made sense to talk about hyperchromia (hyperchromasia); if pale and expressionless - about hypochromia (hypochromasia); the average value is normochromia (normochromasia).
Symptoms
Hypochromia of erythrocytes has several characteristic external manifestations. The problem is that all signs are nonspecific and cannot accurately indicate the presence of this disorder. Symptoms often go unnoticed due to the high intensity of the symptoms of the underlying disease.
Main symptoms:
- headaches and dizziness;
- weakness and fatigue;
- constant drowsiness;
- increased heart rate and shortness of breath;
- irritability and emotional instability;
- coldness of the tips of the fingers and toes;
- excessive pallor of the skin and mucous membranes;
- deformation of the nail plates;
- soreness and bright red tint of the tongue;
- increased hair loss;
- dryness and flaking of the skin;
- slight increase in temperature indicators;
- blood pressure fluctuations;
- change in food preferences or complete aversion to food;
- numbness of the upper and lower extremities;
- hepatosplenomegaly;
- the appearance of “goosebumps” before the eyes;
- problems with concentration.
The clinic is typical for both adults and children.
Symptoms
The clinical picture, the number of manifestations and their severity depend on the stage of the disorder. The longer the process exists, the more signs there are and the more pronounced they are.
A sample list looks like this:
- Pain in muscles, joints, aching bones. Accompanies the patient at all times. The nature may resemble arthritis or myositis, or other specific specific diseases. However, there is no objective data for these diagnoses, which is noticeable during the study. The intensity of pain increases with physical activity. The severity of the discomfort increases as the anemia progresses.
- Weakness, drowsiness, asthenic phenomena. The patient is unable to work normally or perform daily duties. At the same time, even ordinary activity in everyday life becomes an unbearable burden for a person. The only desire is to lie down and rest. Apathy occurs. At night, insomnia is possible, which is an even more painful condition. The use of special drugs can solve the problem, at least partially.
- It is possible to change the shade of the stool to a lighter color. There are also defecation disorders such as constipation and diarrhea. Alternating one and the other in a short period of time (several days). Deviations in the functioning of the digestive tract are typical for various types of anemia and occur almost always. In especially advanced cases, bilirubin may be released into the blood and tissues, causing the skin tone to change to yellow.
- Emotional disorders. The patient becomes irritable and aggressive. Depressed or apathetic. There is no connection with any events. Hot temper can be provoked by the most insignificant phenomena. There is instability of mood, which is manifested by sudden changes in the emotional background within a matter of minutes. If not for seconds. Normal interaction with the patient is difficult.
- Noise in ears. Accompanies insufficient blood circulation to the brain. Nervous tissues and cerebral structures do not receive enough oxygen, which becomes the main cause of the disorder.
- Fainting episodes. Syncope is a serious manifestation of ischemia of brain tissue. Occurs in advanced stages of the disease or in initially severe cases. Urgent correction is needed.
- Perception disorders. First of all visual. Floaters appear in the field of view, photopsia flashes (the simplest hallucinations in the form of bright dots, spots or lines). Possible development of scotomas. Monocular blindness occurs, but is extremely rare.
- Headache. It manifests itself in attacks lasting several hours each. During the day, episodes of discomfort may occur repeatedly. The disorder is characterized by pressure, distension, burning or shooting, pulsation in the parietal, occipital, and frontal regions. Recovery with medication doesn't make much sense. Since the effect is short-term, or even completely absent.
- Disorders of taste preferences. An interesting phenomenon against the background of anemia can be considered a perversion of gastronomic preferences. The patient expresses a desire to consume inedible things. Chalk, chemicals, coal and others.
- Circulatory disorders in the heart muscle. Characterized as angina pectoris. Accompanied by excruciating pain in the chest. A drop in blood pressure levels is also detected. Markings may vary.
- Increased fragility of hair, nails, excess sebum production. There are changes in the cosmetic properties of body tissues. It disappears on its own after the main pathological process is eliminated.
- Dyspnea.
- Disturbance of normal urination.
It is correct to talk not about the symptoms of hypochromia, but about the signs of anemia, iron deficiency or otherwise.
Diagnostics
Modified red blood cells can be detected only after a hematologist deciphers the results of a general clinical blood test. Biological material is collected from a finger. Among the criteria that pay close attention to are:
- color index of red blood cells;
- level of iron-containing protein;
- red blood cell count;
- anisocytosis;
- poikilocytosis.
Changes in the shape of red blood cells
The information obtained will not be able to indicate the root cause, so an integrated approach to studying the condition of the body is necessary. First of all, the clinician must personally perform several manipulations:
- study the medical history - this will help to find out which disease was the basis for the disorder;
- collect and analyze life history - to confirm or refute the influence of physiological sources;
- a thorough physical examination;
- assessment of the condition of the skin and mucous membranes, hair and nail plates;
- measuring blood tone, heart rate and temperature;
- a detailed survey of the patient - to create a complete picture regarding the symptom complex.
In addition, specific laboratory tests, instrumental procedures and consultations with specialists from other fields of medicine will be needed. The diagnostic program is drawn up on a personal basis.
Treatment
To get rid of the disorder, the root cause must be eliminated. Patients will be prescribed individual treatment tactics:
- stopping bleeding using conservative or surgical methods;
- ingestion of iron-containing medications and vitamin complexes;
- blood transfusion - infusion of donor red blood cells into the patient’s blood;
- removal of malignant tumors through surgery, radiotherapy or chemotherapy;
- maintaining a gentle diet;
- physiotherapeutic procedures;
- the use of traditional medicine is permissible only after prior consultation with your doctor.
People with this problem are advised to enrich their menu with products that contain iron. This means that the list of permitted ingredients includes:
- red meats;
- offal;
- seaweed and seafood;
- apples;
- grenades;
- nuts;
- dried fruits;
- egg yolks;
- greenery;
- beet;
- black currant;
- raspberries;
- strawberry;
- kiwi;
- strawberries;
- citrus.
The course of treatment with alternative methods should not last less than 1 month. It is proposed to prepare healing infusions at home based on the following components:
- clover;
- nettle;
- rose hip;
- yarrow;
- berries and leaves of rowan.
Patients will benefit from juices from:
- carrots;
- black radish;
- grenade;
- apple
Prevention and prognosis
To prevent the disorder, people only need to follow a few simple recommendations:
- eat properly and balanced;
- completely give up bad habits;
- avoid blood loss;
- if necessary, take iron supplements and vitamin-mineral complexes;
- promptly treat any pathologies that may cause changes in red blood cells;
- absence of stressful situations;
- undergo a full laboratory and instrumental examination at the clinic several times a year.
The outcome is dictated by the main etiological factor, but is often favorable. Do not forget that in the absence of therapy, the underlying problem worsens - this can lead to the development of complications of a particular disease.
Why is hypochromia dangerous?
Lack of hemoglobin is not a threat to human life. However, if this deficiency is not corrected with appropriate medications, complications may occur. This pathology is more often observed in the elderly generation, which leads to various diseases.
Why is hypochromia dangerous?
During pregnancy, having a lack of hemoglobin is very dangerous, since the fetus will then begin to suffer from oxygen starvation, and it may not survive in the womb. Also, a pregnant woman may experience premature labor, or the child may be born underweight and become weak-minded.
When a danger occurs, the following symptoms may appear:
- the spleen and liver will increase in size;
- an edema condition will occur;
- all limbs will become numb;
- the work of the heart will be disrupted.