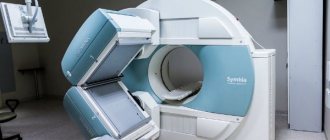
Using an electrocardiographic study, you can assess the condition of the myocardium, its ability to contract and conduct an electrical impulse, and make a diagnosis of rhythm disturbances or enlargement of the heart.
In children, the ECG has differences that are clearly expressed at an early age: a high pulse rate, predominant activity of the right ventricle, a change in the location of impulses. For each period of a child’s formation there are characteristic changes; by the age of 12, the ECG norm for children and adults is the same.
Why do ECGs be done for children?
When examining a child using an ECG, you can determine:
- increased pressure in the pulmonary or systemic circulation;
- heart rhythm and conduction disturbances;
- metabolic disorders in the myocardium - lack of potassium, magnesium or calcium;
- heart muscle strength;
- sufficiency of blood supply to organs;
- is there an enlargement of any part of the heart;
- compliance of indicators with age norms and general development of the body.
This method is not traumatic, is available in any medical institution, does not require prior preparation and cannot harm the child. Therefore, it can be taken without restrictions at any age, starting from the neonatal period. If you analyze the EGC over time, it is easy to assess the effectiveness of the prescribed treatment.
We recommend reading about sinus arrhythmia in a child. You will learn about what respiratory and pathological SA is, the causes and manifestations of rhythm disturbances, diagnosis and treatment. And here is more information about the symptoms and treatment of atrial extrasystole.
Clinical examination: ECG – is it necessary and how often should an electrocardiogram be taken for a child?
Home > Consultations > Children's doctor > Clinical examination: ECG - is it necessary and how often should an electrocardiogram be taken for a child?
Electrocardiography is a method of studying the heart that does not lose its value over the years.
During the procedure, the cardiograph records the electrical potentials that appear during the work of the heart muscle. All information is sent to the doctor in the form of a graph on a paper tape. It is not at all necessary to be ill with something in order to do an ECG of the heart; on the contrary, it will be considered as disease prevention. But it’s no secret that preventing a disease is much easier than treating it.
An ECG is prescribed to children to study the condition and functioning of the heart. Cardiac diagnosis using ECG in children remains the most popular and widespread technique. What explains this?
Firstly, this technique is informative, safe and completely painless, so an ECG can be prescribed even to a newborn child.
Secondly, an ECG of the heart for children does not require any special preparation. The method is surprisingly easy to use and does not force the doctor, the child, or the parents to strain. The very procedure of an ECG performed on an infant does not differ from the ECG of a one-year-old child, or from the ECG of a teenager.
Thirdly, due to the simplicity of the technique, even in a private hospital it will not cost a lot of money - so it is quite accessible to everyone. Everyone can afford to have their child have an ECG.
Fourthly, the speed of the procedure. During the examination, the small patient lies on the couch, electrodes are attached to his chest and limbs, with the help of which an electrocardiogram is recorded. An ECG for children usually lasts no more than 5 - 10 minutes . The procedure usually takes longer only if we are talking about a stress examination or daily monitoring.
Fifthly, the technique monitors the results over time during repeated studies, after which a clinical picture of the diseases, if any, is drawn up. If you have any doubts, you can repeat the ECG after some time to fully clarify the circumstances.
ECG in children has its own characteristics that differ from adult indicators. What explains this?
Each age period is characterized by its own characteristics that must be taken into account during the ECG. Therefore, it is very important that the child’s ECG result is deciphered and explained by an experienced doctor who specializes in functional diagnostics specifically in young patients. ECG indicators in children at newborn age, at one year old, at five years old and in adolescence, for example, may differ ; there is no single norm in this case. The features of a children's ECG are influenced by a number of parameters, including the anatomical position of the heart in the chest, heart rate, autonomic-endocrine factors, changes in the rate of excitation in the myocardium, changes in the ratio of muscle masses of the left and right ventricles, and so on. Thus, throughout the entire process of growth and development of the child, the morphological structure of both blood vessels and the heart is constantly improving, which is reflected in the ECG results. All this is taken into account by the doctor who conducts the ECG, and the interpretation of the results is based on the parameters that should be observed in children of a given age, while the norm can vary and sometimes quite noticeably.
Cardiac automation is well deciphered using an ECG; waves associated with contraction of the atria and ventricles are visible on it; the distance between them makes it possible to estimate the delay time of an impulse moving “from node to node,” and the magnitude of the wave indicates the state of the heart muscle.
The main method for identifying and assessing arrhythmias is ECG . But right away, in order to dispel unnecessary doubts about the ECG of your children, I will note that often when performing an ECG in children, changes such as sinus arrhythmia and isolated incomplete block of the right bundle branch are detected, which are a variant of the age norm. In these cases there is no cause for concern.
Rhythm disturbances in children are often asymptomatic, which makes it difficult to accurately determine the time of their onset. In approximately 40% of cases, arrhythmias are detected by chance (on an ECG) or during examination in connection with a history of acute respiratory viral infection. Children are much less likely than adults to complain of palpitations, a feeling of interruptions in the activity of the heart, and its freezing, even with severe forms of arrhythmia. Along with this, in prepubertal and pubertal age, rhythm disturbances can have a strong emotional coloring, caused by psycho-vegetative disorders, and be accompanied by other cardiac and extracardiac complaints: pain in the heart, increased excitability, sleep disturbances, and meteosensitivity. With arrhythmias, weakness, dizziness and fainting are possible. In newborns and young children, rhythm disturbances can be asymptomatic or severe, with complications. In older children, the prognosis for arrhythmias is usually favorable, but persistent arrhythmias, especially severe forms, can also lead to an unfavorable outcome.
Reasons for testing
Since heart disease is the most common cause of health problems, and their identification in the early stages is the key to successful treatment, indications for testing in a child may include:
- admission to kindergarten or school (scheduled medical examination);
- starting to play sports;
- preparation for surgery;
- previous viral, bacterial infections, sore throat, pneumonia or bronchitis;
- hereditary predisposition to the development of heart disease;
- high blood pressure;
- endocrine disorders;
- retardation in growth and development.
An ECG is necessary in all cases of unexplained weakness and rapid fatigue of the child, pain in the heart, fluctuations in blood pressure, dizziness, shortness of breath and cyanotic skin tone during physical activity.
Electrocardiography: types of diagnostics
The first device capable of recording a high-quality ECG was a string galvanometer designed by V. Einthoven. Its basis was a very thin thread, which was in a magnetic field under a certain voltage. He created a new direction in the physiology of blood circulation - electrophysiology of the heart.
The first such equipment was very bulky and weighed 270 kg.
V. Einthoven identified the main waves, intervals and segments of the ECG, and also calculated their time intervals. He also proposed a system for placing electrodes on the surface of the patient’s body. These data are used by cardiologists to this day.
The jagged edges are the ups and downs of a graph.
. In electrocardiography, a segment is a section of a straight line between two teeth. An electrocardiogram can show cardiac dysfunction in the early stages, as well as consider the possibilities for the development of serious pathologies.
However, an ECG does not always accurately determine the presence of a disease. For example, a disturbance in the rhythm of the heart (arrhythmia) during a study at rest may “lurk” and not manifest itself.
Therefore, the specialist chooses another examination method, there are several of them:
- At rest
is the standard method used most often. The patient lies on the couch in a relaxed state. - With a load
- during this procedure, the doctor will first take electrocardiograph readings, then ask the patient to perform a simple physical exercise (bending, squats), and then examine him again using the device. In addition, it is possible to use other methods - bicycle ergometry and treadmill test. In the first case, a bicycle ergometer is used (a device similar to an exercise bike with varying resistance of the pedals), in the second, a treadmill (a moving track). For each type of examination, electrodes connected to a computer are applied to the patient's body. The doctor monitors and analyzes the readings during the procedure. - Daily (Holter) monitoring
is the longest time-consuming method. When using it, adhesive electrodes are attached to the body of the subject. They are connected to a device that is attached to the belt or worn over the shoulder on a belt. It weighs no more than half a kilogram, so it does not cause any particular inconvenience.
The patient should keep a diary in which he indicates information about changes in physical activity, emotional overload, time of taking medications, sleep and wakefulness. Here he describes pain in the heart area and a feeling of discomfort that can arise during certain activities.
There are two options for Holter monitoring: full-scale and fragmented.
The first continues continuously for 1-3 days, as a result providing accurate and complete information about abnormalities in the functioning of the heart.
Fragmented monitoring may extend over a longer period. It is resorted to only when cardiac dysfunction occurs infrequently. Electrocardiography in this case is carried out using a special device.
To record deviations, the subject turns on the ECG recording button when pain occurs. The apparatus for such research is very miniature: it can be a pocket version or a device in the form of a wristwatch.
A sterile electrode is inserted into the subject's esophagus. This is usually done through the nasopharynx, less often through the mouth. The patient must make swallowing movements. But do not be alarmed - the transesophageal electrophysiological examination of the heart (TECFE) probe is thin and its insertion usually does not cause difficulties. At the same time, electrodes are attached to the chest to record an electrocardiogram.
The electrode is inserted approximately 40 cm - where the heart is closest to the esophagus. After this, they begin to record a cardiogram, and the probe begins to send weak electrical signals to the heart, causing it to contract more often.
At the end of the study, the electrode is removed from the esophagus.
In electrocardiography, there are instrumental methods for studying the functioning of the heart muscle. These include, for example, phonocardiography. In this case, a special microphone records the sounds made when the heart muscle is excited and relaxed. As a rule, listening is carried out by an experienced specialist with good hearing, who is able to separate murmurs and heart sounds from pathological sounds.
The book by V.V. Murashko “Electrocardiography” contains other methods of conducting research. Its cost is low, but it will be very useful for those who want to master the basics of ECG.
How to prepare your child for an ECG
No special preparation is required for the study. It is important that the child is calm and not afraid of doctors and medical personnel. It is best to bring babies after meals or during sleep, when they can calmly respond to others. Parents should explain to older children the day before in the form of a game what will happen during the ECG.
Before visiting the office, you need to think about how it will be convenient to undress the child to apply electrodes to the chest and ankle and wrist joints.
Even children know that an ECG is painless and quick
The electrocardiographic examination lasts about 10 minutes, including placing the patient on the couch. Immediately before the examination, while waiting for your turn in the corridor, you need to rest and catch your breath so that your pulse returns to normal. In the ECG room, you need to free the lower part of your legs and torso from clothing, since the electrodes are applied to the area of the chest, legs and forearms. While recording cardiac activity, breathe as usual, do not be nervous, so as not to distort the results with a high pulse rate. A classic ECG records how the heart works in its normal state - relaxed and at rest.
Rules for conducting an ECG in children at 1 year of age and after
Before the procedure, you need to exclude active games and emotional stress of the child for at least an hour.
After eating, at least 1.5 hours should pass. For young children, special electrodes are used that are firmly attached to the skin without damaging it. For infants, a special cuff belt with fixed sensors can be installed.
After applying the electrodes, newborns are swaddled, and older children need to be persuaded not to make active movements or talk. In order to obtain diagnostically valuable material, it is necessary to register at least 10 - 15 cardiac cycles, and if rhythm disturbances are suspected, there may be more. Therefore, it is advisable that one of the parents be with the small child at all times.
To learn how to take an ECG in a child, watch this video:
How to do an ECG correctly: preparation and conduct of the procedure
For those who do not know how to do an ECG correctly, do not worry: conducting electrocardiography does not require special training. However, some nuances still exist. It is advisable to refrain from eating heavy food 2 hours before the procedure.
Also, do not be nervous, play sports, drink energy cocktails or alcohol, as well as strong coffee or tea. Before the examination, women do not need to apply lotion or cream to the body; they should remove any jewelry from the wrists and chest area: bracelets, rings, chains, etc.
The chest electrodes have a special suction cup that is attached to the body due to the vacuum created. The specialist taking the readings knows very well how to do an ECG correctly, so it is unlikely that he will be able to confuse the wires connecting the suction cups to the device.
Before starting work, the device must be warmed up (3-5 minutes is enough). After this, the position of the recorder pen is adjusted, giving a calibration signal by turning on a special button.
There are no contraindications for conducting an ECG - the study can be performed even on infants.
In this case, the procedure for collecting data from a child is similar to that carried out by adults. Only the result will be different - for example, babies have a higher heart rate.
Some children are afraid of all people in white coats, so they can be very nervous before the procedure. Before it starts, parents should relieve stress in their children - give them a favorite toy, show a funny picture or photo (you can do it on your phone). An older child can be told about the study in advance and shown in a playful way how to do an ECG correctly.
The examination procedure may be difficult for those with complex chest injuries, high obesity, or excessive chest hair - in this case, the electrodes will not adhere tightly to the skin and the examination result will be distorted. The presence of a pacemaker will also lead to incorrect results.
Transesophageal examination cannot be performed in the presence of tumors or other diseases of the esophagus. ECG with stress is contraindicated in acute infectious diseases, chronic heart failure, coronary heart disease, complex rhythm disturbances, and in the acute period of myocardial infarction. Also, you should not do this if there is an exacerbation of diseases of other body systems - urinary, respiratory, digestive.
Decoding of indicators: norm
In a child, the heart is fully formed only during puberty, and the first stage ends at 6–7 years. Therefore, not all deviations from the norm when analyzing a cardiogram should be considered a sign of disease. Correct interpretation can only be carried out by a cardiologist who knows the specific features of each age interval. The teeth are indicated by a Latin letter, and the intervals and segments are indicated by 2 - 3 consecutive letters.
Decoding ECG values
In newborns
The first days of a child’s life pass against the background of an accelerated heart rate from 100 to 160 beats per minute; it is inconsistent. The following changes are typical:
- QRS wave voltage is low;
- the axis of the heart is deviated to the right;
- P (atrial) is relatively large compared to QRS (ventricular), pointed;
- Q may be absent, T is biphasic or negative.
Up to a year
The electrical axis of the heart remains shifted to the right, in most children it approaches a vertical position, the pulse slows down somewhat - to 110 - 115 beats per minute. The following features are considered normal:
- Q is deep in the 3rd standard lead and absent in the right;
- QRS amplitude increases;
- PQ no more than 0.13 s;
- T gradually increases.
All these signs mean a gradual movement of the heart from a horizontal to a vertical position.
From 1 year to 7 years
The heart rate per minute does not exceed 100 beats, the position of the heart is intermediate or vertical. Typical ECG signs:
- PQ within 0.15s;
- QRS high;
- Q are recorded more frequently;
- T becomes positive in lead 3.
- Detection of sinus arrhythmia in children at this age is not a sign of illness From 7 years to 14 years
The amplitude of the waves and the duration of the intervals between them are approaching those in adults, but the pulse rate remains unstable with a tendency to tachycardia, the heart axis occupies a normal position in about half of the children. Arrhythmia of sinus origin of varying severity can be considered a variant of the norm.
ECG devices and the principle of their operation
A cardiograph is a device that records the bioelectric impulses of the heart. The examination result is displayed on thermal paper or display in the form of a graphic curve.
READ Secrets of decoding ECG
This graph is called an “electrocardiogram”. Modern models of cardiographs save the results in electronic form for subsequent computer processing.
An ECG is an informative, relatively inexpensive and accessible test that is done when you need to obtain information about the work of the heart muscle.
Video:
Deviations that an ECG can reveal in children
After deciphering the cardiogram, there may be the following descriptions:
- Sinus rhythm. The norm is that the impulse occurs in the sinus node, as it should be.
- Sinus arrhythmia is considered physiological for children. If it occurs after an infectious disease, it requires observation.
Sinus arrhythmia (9 year old girl)
- Sinus bradycardia - weakness of the sinus node, pulse less than 50 beats, blood supply to organs is disrupted, fainting may occur.
- Sinus tachycardia can occur with high fever, infection, loss of blood or fluid, or anemia.
Sinus tachycardia
- Extrasystole is an extraordinary contraction that occurs with neurosis, hormonal imbalance, myocardial pathology, including myocarditis.
- Paroxysmal tachycardia is an attack of rapid pulse.
Atrial fibrillation is irregular, frequent contractions (350 to 650 beats), blood cannot flow into the ventricles, and from them into the organs. Accompanied by weakness, increased sweating, shortness of breath, and possibly loss of consciousness. Together with atrial flutter, they are the most complex pathology and can lead to dangerous circulatory disorders.
A) Permanent form of atrial flutter in a 6-month-old child; B) Permanent form of atrial fibrillation in a 10-year-old child.
Conduction disturbances are called blockades. In these conditions, the passage of the impulse to contract the heart is inhibited, which is why the ventricles rarely contract. This leads to dizziness, loss of consciousness and seizures in severe cases.
Hypertrophy of the muscle layer develops when parts of the heart are overstrained. Occurs with congenital defects, hypertension, cardiomyopathy. The right ventricle enlarges with lung lesions, Fallot's disease, and septal defects between the ventricles.
We recommend reading about the dangers of sinus arrhythmia. You will learn about normal and irregular sinus rhythm, causes and symptoms of SA, diagnosis, treatment. And here is more information about Wolff-Parkinson-White syndrome.
Benefits of ECG
The main advantages of the study as a diagnostic method:
- Painless.
- Speed: you only have to wait a couple of minutes, and the doctor will spend very little time deciphering.
- Highly informative: the heart is not viewed statically, but in action, which allows one to draw important conclusions about many of its features.
Children, especially small ones, usually do not really like having an ECG, despite the fact that the study brings almost no physical discomfort. It is worth preparing the child for the procedure. It is better if he comes to the examination calm, and not after crying - his emotional state affects the results. Talk to your child, explain to him that this is not scary, it’s even interesting - our specialists will take on further concerns.
What to do if your child is afraid
Often children react with fear to any approach of medical workers, fearing pain. Carrying out an ECG for a small child can be a stress factor, which will affect the reliability of the data obtained. Therefore, you need to know how to calm your baby.
Parental behavior
Young children are greatly influenced by the condition of their parents. In this regard, you need to understand well that an ECG examination is the safest examination method, in which there can be no pain or discomfort for the child.
The only discomfort is the application of a gel that is colder than body temperature. Even frequent ECG recordings do no harm. With their calmness, parents can instill confidence and prevent restless behavior that interferes with ECG readings.
How often can an ECG procedure be done?
Electrocardiography is an inexpensive, accessible and quite informative research method that was invented more than a century ago. Despite such a long period of time, this invention has not lost its relevance and, moreover, continues to be improved to this day, which indicates its relevance.
Using this method, you can not only detect heart rhythm disturbances, but also assess the condition of the myocardium. Our article will tell you in detail about the features of the study and how often an ECG can be done.
How does an electrocardiograph work?
An electrocardiograph records cardiac electrical potentials. The cardiogram is recorded using electrodes attached to the body of the subject. The main components of this device include:
- system responsible for increasing heart rate;
- galvanometer;
- registrar;
- switch.
The electrocardiograph receives a weak electrical impulse from the heart muscle, which occurs in the patient. Next, it is sensed by the electrodes, after which it is amplified and captured by a galvanometer. Any change in the electromagnetic field is recorded and then recorded by recorders on a paper tape that moves evenly.
The result is a kind of graph displaying the work of the cardiac departments. It is expressed in teeth of different sizes. The length of the graph depends on how strong the signal comes from a particular department. The electrocardiograph does not interfere with the functioning of the body, it simply records the work of the heart.
In addition, this device does not emit ionizing radiation, which is observed in computer tomographs, radiographic units, and does not generate magnetic fields, like a magnetic resonance tomograph. The operation of this device is based on recording electrical potentials created by the heart muscle and producing a cardiogram, which is deciphered by specialists.
Variant of normal ECG
After which the cardiologist gives an opinion on the work of the heart muscle and its condition. Based on this, it is important not only to correctly record, but also to decipher the resulting recording.
Over the course of a long time, through experimentation, a standard was established that a particular tooth height should meet; any deviation indicates the presence of a certain problem.
Only by correctly deciphering the result can you accurately diagnose the patient.
Is it possible to do an ECG often?
Based on the foregoing, we can make a well-founded conclusion that this examination does not belong to the category that is harmful to the health of the body.
Since it only measures heart rate, it does not emit radiation at all and does not have any effect on human health.
In addition, there are professions where people constantly experience severe stress and, in connection with this, they undergo electrocardiography daily, which proves the complete safety of this study.
Many people have the opinion that if the device is allowed to examine children and pregnant women, then it is harmless.
And this is true, since pregnant women and children under 14 years of age are among the most vulnerable categories.
This is due to the fact that the child’s body and the growing fetus are quite susceptible to any adverse effects. ECGs are allowed for these categories, and only as many as are needed to clarify the diagnosis.
Important! An ECG can be done even several times a day; it will not cause the slightest harm to the body.
Unfortunately, modern life is characterized by a serious rhythm, and therefore the mortality rate, which is caused by cardiovascular diseases, is increasing. Therefore, the most reliable way of early diagnosis is this examination method.
The attending physician decides how often an ECG should be done, taking into account the individual characteristics and medical history of the patient. When examining electrocardiography, you can use the principle “more often is better than less often.” However, there is no point in conducting research every day.
Medicine has the following recommendations in this regard:
- A healthy adult is allowed to have an ECG of the heart no more than once a year;
- if the profession involves professional risks, then it is advisable to do the research every six months;
- for professional athletes, the frequency of diagnostics is controlled by a sports doctor;
- Elderly people can be examined more often, at least once every 3 months.
Athletes are often prescribed a stress ECG
The frequency of an electrocardiogram, unlike research methods that are harmful to human health, does not have an exact limit on its number. For preventive purposes, an ECG must be done at least once a year, this is especially true for people who have crossed the 40-year mark.
In what cases does a pregnant woman need to have an ecg done frequently?
Based on the standards, a pregnant woman is tested one-time when she registers. However, if there are any complaints or suspicions of cardiac pathologies, the doctor can send the expectant mother for examination as long as necessary. Typically, among the reasons influencing the increase in the number of ECGs are the following:
Right ventricular hypertrophy on ECG
- changes in blood pressure;
- fainting;
- dizziness;
- presence of pain in the left breast area;
- rapid heartbeat;
- the appearance of shortness of breath;
- long-term toxicosis.
In addition, this diagnostic can be carried out in any quantity during any month of pregnancy; it is completely safe for both the woman and the baby.
Analysis order
For a more detailed examination of the heart, an ECG analysis is performed, as well as a calculation of the area of the teeth.
This is done using special leads; in addition, the necessary results can be obtained if you use such an indicator as the direction of the electrical axis.
In this case, the total QRS vector is used, and in conclusion its direction must be indicated: horizontal or vertical.
ECG analysis must be carried out only in a sequential order, in which all deviations from the norm present in the work of the heart muscle can be identified.
A more rigorous interpretation of the ECG is made by analyzing and calculating the area of the teeth using special leads (vector theory), however, in practice, they mainly make do with such an indicator as the direction of the electrical axis, which represents the total QRS vector.
It is clear that everyone’s chest is structured differently and the heart does not have such a strict arrangement, the weight ratio of the ventricles and the conductivity inside them are also different for everyone, therefore, when deciphering, the horizontal or vertical direction of this vector is indicated.
Doctors carry out ECG analysis in a sequential order, determining the norm and violations:
- Assess the heart rhythm and measure the heart rate (with a normal ECG - sinus rhythm, heart rate - from 60 to 80 beats per minute);
- Intervals (QT, norm – 390-450 ms) are calculated, characterizing the duration of the contraction phase (systole) using a special formula (I often use Bazett’s formula). If this interval lengthens, then the doctor has the right to suspect ischemic heart disease, atherosclerosis, myocarditis, rheumatism. Hypercalcemia, on the contrary, leads to a shortening of the QT interval. The conductivity of the pulses reflected through the intervals is calculated using a computer program, which significantly increases the reliability of the results;
- The position of the EOS begins to be calculated from the isoline along the height of the teeth (normally R is always higher than S) and if S exceeds R and the axis deviates to the right, then they think about disturbances in the activity of the right ventricle, if on the contrary - to the left, and the height of S is greater than R in II and III leads – left ventricular hypertrophy is suspected;
- The QRS complex is studied, which is formed during the conduction of electrical impulses to the ventricular muscle and determines the activity of the latter (the norm is the absence of a pathological Q wave, the width of the complex is not more than 120 ms). If this interval shifts, then we speak of blockades (full or partial) of the bundle branches or conduction disturbances. Moreover, incomplete blockade of the right bundle branch is an electrocardiographic criterion of right ventricular hypertrophy, and incomplete blockade of the left bundle branch may indicate left ventricular hypertrophy;
- They describe the ST segments, which reflect the period of restoration of the initial state of the heart muscle after its complete depolarization (normally located on the isoline) and the T wave, which characterizes the process of repolarization of both ventricles, which is directed upward, asymmetrical, its amplitude is lower than the wave in duration and is longer than the QRS complex.
The decoding work is carried out only by a doctor, however, some ambulance paramedics perfectly recognize common pathologies, which is very important in emergency cases. But first, you still need to know the ECG norm.
This is what the cardiogram of a healthy person looks like, whose heart works rhythmically and correctly, but not everyone knows what this record means, which can change under various physiological conditions, such as pregnancy.
In pregnant women, the heart takes a different position in the chest, so the electrical axis shifts. In addition, depending on the duration, the load on the heart is added.
An ECG during pregnancy will reflect these changes.
The cardiogram indicators in children are also excellent; they will “grow” with the baby, and therefore will change according to age; only after 12 years, the child’s electrocardiogram begins to approach the ECG of an adult.
Carrying out an ECG
When electrocardiography is performed, sensors are connected to the patient's body that record the electric field. The pulses enter the device, after which the data is recorded in graphical form. The information obtained is called a cardiogram.
A pediatric ECG is necessary to identify possible congenital pathologies. The study is carried out at different age periods, this can be an ECG of a newborn in a maternity hospital or in a clinic in the first year of life. As the child gets older, electrocardiography is prescribed if symptoms appear that may indicate heart pathologies.
Before the examination, the child is undressed, exposing the chest, legs and arms, and then placed on the couch. If an ECG is performed on a child at 1 year of age or before one year, then the mother needs to remain nearby. Electrodes are placed on the wrists, legs and chest. An ECG of the heart is performed quickly, the procedure takes 5-15 minutes.
ECG for children
Indications
A pediatric ECG should be performed before discharge from the hospital. This procedure is mandatory due to the possibility of a child being born with heart defects.
Doctors advise conducting a study if the baby has the following symptoms:
- extraneous heart sounds are heard;
- dizziness often occurs;
- there were cases of fainting;
- fatigue uncharacteristic for age was noted;
- pain in the thoracic region;
- frequent ARVI, bronchitis, pneumonia;
- swelling of the limbs.
The described signs often signal a malfunction of the heart or pathology of other internal organs. To exclude complications of diseases, it is necessary to carry out timely diagnostics, in this case an ECG, although the doctor may prescribe other research methods.
No special preparation methods are required to conduct a pediatric ECG. 2-3 days before the procedure, it is worth making sure that the baby is in a stable psychological state. To do this, you will need to eliminate stressful situations and various experiences. Parents will need to explain to their child the essence of the procedure and the purpose of it.
So that the child is not afraid of the doctor, it is recommended to simulate the situation at home, in other words, to play doctor and patient with the child. Due to this, it will be possible to visualize the procedure and the method of its implementation. In addition, it is allowed to show a video of the study. Children under 1 year of age are allowed to perform an ECG in their sleep, but this is often rarely done.
Important! Morale must be normal to obtain reliable ECG results. Maximum information content depends on the child’s calmness.
Features of the diagnostic method
The ECG method has been successfully used in medical practice for more than one hundred and fifty years. Of course, over all these years it has undergone significant changes, but the principle and algorithm for taking heart readings remains unchanged.
The main essence of the ECG method is to record electrical impulses that come from the heart muscle through a special device.
A cardiogram shows the sinus rhythm of the heart, the analysis of which allows us to get the most complete picture of the general state of human health.
The results of the heart function obtained after the ECG are compiled into a final conclusion.
If deviations from the norm are detected in the functioning of the heart, the doctor makes a diagnosis and decides to prescribe therapeutic therapy.
An ECG can be performed in adults and children; in addition, this diagnosis is considered routine in pregnant women.
Currently, every ambulance team has a portable electrocardiograph, which allows doctors to quickly identify pathologies in the heart and, if necessary, transport the patient to the hospital in a timely manner.
The cardiogram itself consists of all sorts of teeth, which are not understandable to everyone, left on a paper tape by a recorder.
Meanwhile, many patients try to independently learn to recognize the main indicators in the work of the heart muscle, but this cannot be done without special training.
In order to independently learn how to analyze the readings of a cardiac graph and read sinus rhythm, you must first form an accurate idea of how the human heart functions.
The human heart muscle consists of four separate chambers called the atria and ventricles.
Specifics of the examination
In the process of diagnosing various childhood diseases, one of the important aspects is the registration of an electrocardiogram, even if there are no symptoms of heart damage. If we consider in general the interpretation of the ECG of an adult and a child, then there are no particular differences in them. However, it should be noted that the gradual anatomical and physiological changes that occur with the baby from the moment of his birth until he reaches adolescence are all reflected in the indicators.
ECG interpretation in children analyzes the following parameters:
- regularity of heart contractions;
- frequency;
- axis location;
- electrical impulse conductivity level;
- depth/width of column P in the interval PQ;
- feature of the QRST tooth complex;
- parameters of the QT interval and RS-T segment.
ECG in a newborn during the first two days of life
In ECG in children
During the first two days, individual fluctuations are noted.
Immediately after birth, the heart rate is 157 per minute, and after cutting the umbilical cord - 142 per minute. In the first hours after birth, doctors note fluctuations in the RR interval from 0.44 to 0.54″, the heart rate is 123.0±1.8 per minute. To perform an ECG on an infant,
it is important to swaddle him well. This is necessary to ensure that the recording of the electrocardiographic curve is correct. The child should be warm and motionless. Swaddling is abandoned only if the child is in serious condition and practically does not move. It is recommended to record an ECG 1.5-2 hours after feeding and before X-ray examinations and physical procedures.
Where can I get an ECG for a child in Moscow?
If your child has received a referral for an ECG, then this is not a reason to panic. The procedure is completely painless and will not take more than 10 minutes. Research is carried out using modern technology and gives very accurate results. ECG in children
has many features. Our clinic specialists have extensive experience in reading cardiograms. The Medicine Clinic is accredited according to the most stringent American standards of medical care and is ready to provide you with:
- diagnostics using the latest equipment, which is used in the best clinics in Europe;
- service at the level of foreign medical centers;
- consultations and treatment from the best specialists in Europe and Russia.
In the modern clinic "Medicine" you can do a paid ECG for your child
and order a transcript from an experienced cardiologist. You will receive reliable information about your baby’s health condition and, if necessary, receive timely treatment.
An ECG for children is performed in the same way as for adult patients. The process is completely painless, short and safe. Using it, you can find out the regularity of heart contractions, their frequency, and notice deviations in the metabolism of electrolytes: potassium, calcium and magnesium. The result is recorded on paper tape as a graphic recording of the electrical activity of the heart. Information is read from the surface of the body using small suction cup sensors, the size and shape of which depend on the client’s age. The study can be carried out many times, which is important for small patients who need to monitor the work and development of the heart over time.
Don't panic if your baby has a rapid heart rate. The normal rate for infants is 130-140 beats per minute. Indicators decrease only by adolescence (up to 60-80 beats). In addition, children are more susceptible to various environmental changes and moods, so the heart beats more often when crying, anxiety, elevated body temperature, or physical stress.
Children do not suffer from intoxication and chronic infections like adults. But schoolchildren often experience hypertension, rheumatic heart disease and cardiac arrhythmia. Recently, there are more and more young patients with vegetative dystonia, arterial hypertension, cardiomyopathy and other disorders of the cardiovascular system.
The causes of these diseases in children (except for congenital defects) are a sedentary lifestyle, improper daily routine, stress, unhealthy diet, etc.
How to take an ECG correctly
The technique for performing electrocardiography has a simple procedure and is carried out in stages:
- patient preparation;
- application of electrodes;
- recording bioelectrical activity on paper;
- deciphering the results.
It is important not to confuse the electrodes, but to check the device for serviceability before use.
A video about the ECG recording technique was filmed by the channel - OFFICIAL TNU.
To record standard and enhanced leads, three electrodes (red, yellow and green) are used, which are placed on the arms and left leg and form an Einthoven triangle. The black electrode, which is placed on the right leg, grounds the system.
You need to set them like this:
- red - right hand;
- yellow - left hand;
- green - left leg;
- black - right leg.
To record the chest leads, one or six pear-shaped electrodes are used (depending on the type of cardiograph).
How to place chest electrodes:
- lead V1 - in the IV intercostal space along the right edge of the sternum;
- lead V2 - in the IV intercostal space along the left edge of the sternum;
- lead V3 - between the second and fourth positions;
- lead V4 - in the 5th intercostal space along the left midclavicular line;
- lead V5 - at the same horizontal level as V4, along the left anterior axillary line;
- lead V6 - along the left midaxillary line at the level of V4.5.
Scheme for applying chest electrodes
For convenience, all electrodes have their own color.
The location of the four main ones is easy to remember from a traffic light or from a funny reminder “Every Woman Is Meaner Than the Devil.”
In a single-channel cardiograph, one white bulb is used to take chest leads on an ECG.
- V1 - red;
- V2 - yellow;
- V3 - green;
- V4 - brown;
- V5 - black;
- V6 - blue.
Lead diagram
When recording an ECG, 12 standard leads are currently used: 6 from the limbs and 6 from the chest.
Each of the 6 leads shows one or another part of the heart.
On standard leads:
- I - anterior cardiac wall;
- II - posterior cardiac wall;
- III - their totality.
Diagram of standard limb leads
On reinforced leads:
- aVR - lateral cardiac wall on the right;
- aVL - lateral cardiac wall anterior to the left;
- aVF - posterior inferior wall of the heart.
Scheme of reinforced limb leads
On the chest leads:
- V1 and V2 - right ventricle;
- VZ - septum between the two ventricles;
- V4 - upper cardiac section;
- V5 - anterior lateral wall of the left ventricle;
- V6 - left ventricle.
Chest lead diagram
This simplifies the task of diagnosing diseases. Changes in each lead characterize the pathology in a certain area of the myocardium.
Deviations that often occur
The normal ECG in children shows that sometimes a seemingly correct sinus rhythm can be interrupted by certain disturbances, which in turn are signs of a pathological process in the body. If frequent changes of this kind are observed, then it is very important to correctly assess the range of heart rate fluctuations and establish their relationship with other symptoms. Changes in heart rhythm are quite common, and sometimes they are completely benign.
As for the P-P interval, its changes are observed in almost all children. Their severity in some cases indicates an irregular working rhythm of the heart. To confirm sinus arrhythmia, first of all, you need to establish a connection with the phases of breathing, namely: exhalation rhythm slows down, inhalation speeds up.
Interesting! 50% of all newborns experience episodes of sudden prolongation of the P-P interval. The older the child, the less frequently this occurs and, as a rule, only in isolated cardiac cycles.
Some deviations may be expressed in the duration of the QRS complex, the QT interval, and the presence of extrasystoles.
ECG interpretation
The cardiography method was first used at the beginning of the 19th century. At this time, scientists found out that heart impulses could be recorded on paper using the then-invented cardiograph. But this process took too long.
Normal indicators in children
The electrocardiogram is a linear graphic form that expresses the size of the waves and the duration of the phases of the cardiac cycle. ECG interpretation requires careful analysis of all values.
Heart rhythm is one of the most important components in the work of the heart.
The main muscle of the body works without interruption and creates sinus rhythm. This rhythm is determined by the beating of the heart in equal fractions of time - seconds. When the heart rhythm is abnormal, arrhythmia occurs.
Conduction is the ability of the heart to conduct impulses from the sinus node to the myocardium. The heart is surrounded by nerve fibers that send electrical impulses.
Waves, ECG segments
Photo: https://pixabay.com/illustrations/heartbeat-pulse-healthcare-medicine-163709/ As we have already found out, an ECG is a linear line that displays heart performance indicators.
On this line we see “hills”, which are called teeth. There are only five of them and they are designated by Latin letters - P, q, r, s, t. The first wave rising above the line is the P wave. It reflects the beginning of the atria.
Cardiac depolarization is a process that reflects excitation or activation of the heart muscle. Repolarization is the process of relaxation of the heart muscle.
Thus, the P wave reflects the process of depolarization of the right and left atrium.
The next wave is Q. It tells us about the excitation of the middle part of the interventricular septum. The area from the P wave to the Q wave is called a segment. The segment displays the spread of excitation along the nerve fibers of the heart.
Wave R - depolarization of the walls of the left and right ventricles.
The S wave is the excitation of the ventricles and interventricular septum.
The ST segment is the time of complete coverage of excitation of the ventricular myocardium.
The T wave characterizes the repolarization of the ventricular myocardium.
The ECG film in each lead must have at least 4 cardiac complexes.
ECG waves
To assess the condition of the child and his heart, special designations of teeth in the form of Latin letters are used. The table shows the ECG wave interpretation:
| Designation | Decoding |
| T wave | Shows relaxation of the ventricles. |
| P wave | Shows contraction and relaxation of the atria. |
| Q wave and S wave | They talk about excitation of the septum between the ventricles. |
| R wave | Indicates the excitation of the ventricles of the heart. |
The PQ interval measures the time it takes for an impulse to travel from the atria to the ventricles.
The following segments are distinguished on the cardiogram:
- TR – relaxation of the myocardium in the interval between two contractions;
- ST – peak of ventricular excitation;
- QRST is the time of one ventricular contraction.
The indicators described are considered basic, but doctors can use other types of designations.
The right ECG shows right ventricular hypertrophy. In this case, the R wave on the graph is high, and the S wave is deep and exceeds it in amplitude. This is called S-type ECG. For newborns, the spelling is normal.
After the ECG, the doctor receives a cardiogram and if no pathologies are detected, the indicators will be as follows:
- Heart rate in children 1-3 years old is 100-110 beats, for children 3-5 years old – 100 beats, children 6-8 years old – up to 90 beats. 9-12 years – 70-85 beats.
- The QRS wave interval is up to 0.1 s.
- Wave P – no more than 0.1 s.
- The PQ wave interval is about 0.2 s.
- The QT wave interval is up to 0.4 s.
Q wave
It is worth noting that study indicators may vary due to certain characteristics. In addition, the value may be influenced by the time of the ECG, the general condition of the person, and the correct application of the sensors.