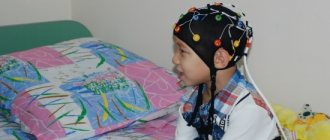
The importance of the normal functioning of parts of the brain is undeniable - any deviation will certainly affect the health of the entire body, regardless of the person’s age and gender. Therefore, at the slightest signal of a violation, doctors immediately recommend undergoing an examination. Currently, medicine successfully uses a fairly large number of different methods for studying the activity and structure of the brain.
But if it is necessary to find out the quality of the bioelectrical activity of its neurons, then the electroencephalogram (EEG) is clearly considered the most suitable method for this. The doctor performing the procedure must be highly qualified, since, in addition to conducting the study, he will need to correctly read the results. Competent interpretation of the EEG is a guaranteed step towards establishing the correct diagnosis and subsequent prescription of appropriate treatment.
More about the encephalogram
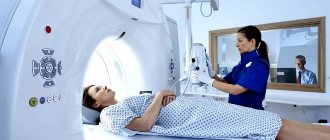
The essence of the examination is to record the electrical activity of neurons in the structural formations of the brain. An electroencephalogram is a kind of recording of neural activity on a special tape using electrodes. The latter are attached to areas of the head and record the activity of a certain area of the brain.
The activity of the human brain is directly determined by the work of its midline formations - the forebrain and the reticular formation (connecting neural complex), which determine the dynamics, rhythm and construction of the EEG. The connecting function of the formation determines the symmetry and relative identity of signals between all brain structures.
The structure of the brain, based on these data, the specialist deciphers the diagnosis
The procedure is prescribed if there are suspicions of various disorders of the structure and activity of the central nervous system (central nervous system) - neuroinfections such as meningitis, encephalitis, poliomyelitis. With these pathologies, the activity of the brain changes, and this can be immediately diagnosed on the EEG, and in addition, the localization of the affected area can be established. An EEG is carried out on the basis of a standard protocol, which records measurements taken while awake or asleep (in infants), as well as using specialized tests.
The main tests include:
- photostimulation - exposure of closed eyes to bright flashes of light;
- hyperventilation - deep, rare breathing for 3-5 minutes;
- opening and closing eyes.
These tests are considered standard and are used for encephalograms of the brain in adults and children of any age, and for various pathologies. There are several additional tests prescribed in individual cases, such as: clenching your fingers into a so-called fist, staying in the dark for 40 minutes, depriving yourself of sleep for a certain period, monitoring night sleep, and passing psychological tests.
These tests are determined by a neurologist and are added to the main tests performed during the examination when the doctor needs to evaluate specific brain functions.
How often should the study be repeated?
If the diagnosis has not shown significant changes in brain electrical activity, then a repeat film in the absence of new symptoms may not be removed.
When identifying foci, the encephalogram will become the main objective diagnostic criterion for the effectiveness of the prescribed therapy.
EEG can be performed as many times as necessary
The study must be repeated at least every year. Assessing the dynamics will allow you to adjust therapy to prevent the resumption of attacks (increasing or decreasing doses of antiepileptic drugs).
Even after the diagnosis of epilepsy is removed, it is necessary to repeat the encephalogram for another 3-5 years to prevent relapse. After surgery, annual examination is also recommended for several years. This will avoid many complications.
What can be assessed with an EEG?
This type of examination allows you to determine the functioning of parts of the brain in different states of the body - sleep, wakefulness, active physical, mental activity and others. EEG is a simple, absolutely harmless and safe method that does not require disruption of the skin and mucous membrane of the organ.
Currently, it is widely in demand in neurological practice, since it makes it possible to diagnose epilepsy and highly identify inflammatory, degenerative and vascular disorders in the brain. The procedure also provides identification of the specific location of tumors, cystic growths and structural damage as a result of trauma.
EEG using light and sound stimuli makes it possible to distinguish hysterical pathologies from true ones, or to identify simulation of the latter. The procedure has become almost indispensable for intensive care units, providing dynamic monitoring of comatose patients.
The disappearance of eclectic activity signals on the EEG indicates the onset of death
What are the features of the EEG procedure?
Taking into account the child’s age, the procedure for conducting encephalography is selected. If the baby is very small, then he can lie in his mother’s arms or on the changing table. The most important thing is that he sleeps. The entire procedure will take no more than 20 minutes, because brain activity is recorded during the sleep period.
Older children sit on a couch or in a chair; their head should be straight, it should not be tilted forward so that its readings are distorted. A small patient should behave calmly during the examination. EEG is done a little differently for older children. The procedure involves more complex studies and may therefore take much longer.
Process of studying the results
The analysis of the results obtained is carried out in parallel during the procedure, and during the recording of indicators, and continues after its completion. When recording, the presence of artifacts is taken into account - mechanical movement of electrodes, electrocardiograms, electromyograms, and induction of mains current fields. The amplitude and frequency are assessed, the most characteristic graphic elements are identified, and their temporal and spatial distribution is determined.
Upon completion, a patho- and physiological interpretation of the materials is made, and on its basis an EEG conclusion is formulated. Upon completion, the main medical form for this procedure is filled out, called a “clinical electroencephalographic report”, compiled by a diagnostician based on the analyzed data from the “raw” recording.
The transcript of the EEG conclusion is formed on the basis of a set of rules and consists of three sections:
- Description of the leading types of activity and graphic elements.
- Conclusion after description with interpreted pathophysiological materials.
- Correlation of indicators of the first two parts with clinical materials.
The main descriptive term in EEG is “activity”, it evaluates any sequence of waves (sharp wave activity, alpha activity, etc.).
Where to do an EEG for a child
This procedure can be done in a medical institution that has the appropriate equipment and specialists to carry it out. Despite the fact that the process of examining children and adults is practically no different, the doctor is required to have additional knowledge in the field of pediatric encephalography.
As for the capital of Russia, an EEG for a child in Moscow can be done at a medical clinic. The medical institution has all the necessary equipment, the most modern, and there are specialists in conducting children's EEG. Experienced doctors have enough knowledge to decipher the results, and will also quickly find a common language with the baby.
Do not be afraid of modern research, including encephalography. It is better to detect deviations in a timely manner and take appropriate measures than to treat the suspected disease for a long time without results.
Types of human brain activity recorded during EEG recording
The main types of activity that are recorded during the procedure and subsequently subjected to interpretation and further study are wave frequency, amplitude and phase.
Frequency
The indicator is estimated by the number of wave oscillations per second, recorded in numbers, and expressed in a unit of measurement - hertz (Hz). The description indicates the average frequency of the activity being studied. As a rule, 4-5 recording sections with a duration of 1 s are taken, and the number of waves in each time interval is calculated.
Amplitude
This indicator is the range of wave oscillations of the eclectic potential. It is measured by the distance between the peaks of waves in opposite phases and is expressed in microvolts (µV). A calibration signal is used to measure the amplitude. If, for example, a calibration signal at a voltage of 50 µV is determined on a record with a height of 10 mm, then 1 mm will correspond to 5 µV. In deciphering the results, interpretations are given to the most common meanings, completely excluding rare ones.
Phase
The value of this indicator evaluates the current state of the process and determines its vector changes. On the electroencephalogram, some phenomena are assessed by the number of phases they contain. Oscillations are divided into monophasic, biphasic and polyphasic (containing more than two phases).
Rhythms of brain activity
The concept of “rhythm” in the electroencephalogram is considered to be a type of electrical activity related to a certain state of the brain, coordinated by appropriate mechanisms. When deciphering the EEG rhythm indicators of the brain, its frequency corresponding to the state of the brain region, amplitude, and its characteristic changes during functional changes in activity are entered.
Characteristics of brain rhythms depend on whether the subject is awake or asleep
Periodic diffuse epileptiform discharges
Electrical discharges in this type of generalized changes in BEAGM occur at regular intervals. The discharges are multiphase and have an epileptiform morphology. Thus, they are similar to periodic lateral epileptiform discharges (PLEDs), except that they have a generalized rather than lateral distribution.
They are sometimes called generalized periodic epileptiform discharges (GPED). In contrast, the term bi-PLED generally refers to periodic discharges that are asynchronous.
Burst-suppression pattern or mild periodic EEG changes
Moderate regulatory changes in the EEG are characterized by a burst of activity (a mixture of sharp and slow waves), periodically alternating with episodes of inhibition (activity <10 μV). As a rule, episodes of inhibition are longer (usually 5-10 s) than bursts of activity (1-3 s). In some patients (for example, a child), the change in excitation and inhibition of the cerebral cortex can occur very quickly.
Appearance of pathological EEG, “burst-suppression” pattern
Electrobrain inactivity
Electrobrain inactivity (EMI) is characterized by activity less than 2 μV; To make a diagnosis of brain death, the electroencephalogram must be recorded according to strict rules. These requirements determine recording time, interelectrode distance, test reactivity, and recording continuity.
Severe encephalopathic electroencephalogram patterns are nonspecific with respect to etiology, but represent extremely dangerous degrees of encephalopathy. Because sedatives may cause or worsen these abnormalities, interpretation of the findings should only be performed by a neurologist. The above types of generalized disorders indicate very severe brain dysfunction if sedatives are excluded as a cause.
Intermittent discharges, including burst-suppression patterns, are somewhat more common in anoxic injuries than in other systemic disorders. Intermittent epileptiform discharges may be caused by high doses of sedatives such as barbiturates, benzodiazepines, or propofol.
In the appropriate clinical context, certain periodic patterns may aid in the diagnosis of Creutzfeldt-Jakob disease (CJD) and subacute sclerosing panencephalitis (SSP). Classically, the periodicity for CJD is approximately 1-2 seconds, while for PSP it is about 4-10 seconds.
Rhythmicity or periodicity is one of the hallmarks of electrographic seizures; Thus, paroxysmal discharges are quite often observed in the structure of pseudoepileptic seizures.
Attention! EMR may be the basis for a diagnosis of clinical death. However, contrary to popular belief, an EEG is not required for a neurologist to conclude brain death and is only used as an auxiliary test.
Rhythms of a waking person
Brain activity recorded on the EEG in an adult has several types of rhythms, characterized by certain indicators and states of the body.
Preparing for an EEG of the brain
- Alpha rhythm. Its frequency remains in the range of 8–14 Hz and is present in most healthy individuals – more than 90%. The highest amplitude values are observed when the subject is at rest, in a dark room with his eyes closed. It is best identified in the occipital region. It is fragmentarily blocked or completely subsides during mental activity or visual attention.
- Beta rhythm. Its wave frequency fluctuates in the range of 13–30 Hz, and the main changes are observed when the subject is active. Pronounced fluctuations can be diagnosed in the frontal lobes under the obligatory condition of active activity, for example, mental or emotional arousal and others. The amplitude of beta oscillations is much less than alpha.
- Gamma rhythm. The oscillation interval is from 30, can reach 120–180 Hz and is characterized by a rather reduced amplitude - less than 10 μV. Exceeding the limit of 15 μV is considered a pathology causing a decrease in intellectual abilities. Rhythm is determined when solving problems and situations that require increased attention and concentration.
- Kappa rhythm. It is characterized by an interval of 8–12 Hz, and is observed in the temporal part of the brain during mental processes by suppressing alpha waves in other areas.
- Lambda rhythm. It has a small range - 4–5 Hz, and is triggered in the occipital region when it is necessary to make visual decisions, for example, when searching for something with open eyes. The vibrations disappear completely after concentrating your gaze on one point.
- Mu rhythm. Defined by the interval 8–13 Hz. It starts in the back of the head, and is best observed in a calm state. Suppressed when starting any activity, not excluding mental activity.
Other EEG rhythms and their characteristics
In addition to the basic electrical impulses of brain activity, there are other waves that are used to study the patient's condition much less frequently. But in some cases, they can also influence the identification of the cause of the disease. These include:
- Gamma pulse. Oscillations 30-120(170) Hz with an amplitude of up to 10 microvolts. An increase in the latter above 15 μV is regarded as a pathology. Activation of the gamma rhythm occurs when solving problems of increased complexity, those that require special attention and concentration. According to some theories, gamma waves are interconnected with the work of consciousness. A number of researchers associate gamma rhythm disturbances with schizophrenia.
- The mu rhythm is impulse signals that have the same frequency as the ɑ rhythm, but are recorded in the central parts of the brain. Their activation occurs with tactile stimuli, mental activity, and expression of emotions.
- Lambda rhythm - manifests itself when the gaze follows an object. Localized in the posterior brain regions. Frequency 4-5 Hz. Disappears as soon as the subject fixes his gaze on any fixed point.
- Kappa rhythm – fluctuates in the ɑ-range. It is noted in the anterior temporal regions. Its amplitude does not exceed 20-30 microvolts. Occurs when ɑ waves are suppressed during mental activity.
- Pi rhythm is a slow oscillation of 3-4 Hz recorded in the posterior regions of the brain.
- The phi rhythm is fixed in the delta range. Localized in the back of the brain. Occurs when closing the eyes.
- Sigma rhythm. Pulses with a frequency of 10-16 Hz (most often 12-14 Hz). The amplitude of oscillations in adults usually does not exceed 50 μV. It appears in the initial stage of slow-wave sleep, following the state of drowsiness.
With the active action of delta waves, the sigma rhythm is practically absent (with rare exceptions). Σ waves are present during the transition to the REM sleep stage, but in the advanced phase this stage is completely blocked.
Rhythms in sleep
A separate category of types of rhythms that manifest themselves either in sleep conditions or in pathological conditions includes three varieties of this indicator.
- Delta rhythm. Characteristic of the deep sleep phase and for comatose patients. It is also recorded when recording signals from areas of the cerebral cortex located on the border with areas affected by oncological processes. Sometimes it can be recorded in children 4–6 years old.
- Theta rhythm. The frequency interval is within 4–8 Hz. These waves are triggered by the hippocampus (information filter) and appear during sleep. Responsible for high-quality assimilation of information and forms the basis of self-learning.
- Sigma rhythm. It has a frequency of 10–16 Hz, and is considered one of the main and noticeable oscillations of the spontaneous electroencephalogram, which occurs during natural sleep at its initial stage.
Based on the results obtained during EEG recording, an indicator is determined that characterizes a complete all-encompassing assessment of the waves - bioelectrical activity of the brain (BEA). The diagnostician checks the EEG parameters - frequency, rhythm and the presence of sharp flashes that provoke characteristic manifestations, and on these grounds makes a final conclusion.
How to do an EEG for children
There are several types of procedure:
- routine;
- sleep;
- with deprivation.
In all cases, the study is carried out in the same way; it includes three stages.
- Preparatory. Placing the subject on a couch or chair, applying a special gel, attaching electrodes.
- Basic. Actually, research. Darkening the room, turning on the device, video monitoring (VEM) of the patient’s movements.
- Final. Decoding the result.
Preparing the child
It is very important that the patient remains calm during the procedure. The day before the diagnosis, it is better to give up TV and computer, replacing them with calmer activities. You can take a walk in the park away from the bustle.
You should not drink a lot of liquid.
On the eve of the study, the baby should not eat chocolate, drink a lot of tea and sparkling water. Sweet and salty foods should be limited. Before the session, the child can be fed tasty food so that he does not become capricious, but no later than two hours before the start of the examination.
The little patient's hair should be washed well with shampoo. You need to remove all metal objects from your head.
If the baby is breastfed, the mother must express milk to take with her. Artificialists should also prepare a bottle of the mixture.
Proper psychological preparation is extremely important. Sometimes children are afraid of doctors; a cap with electrodes can also frighten them. You can tell your child that this is a magic helmet that will turn him into a superhero. The children's procedure goes without problems if the parents show that there is nothing to be afraid of, it is just an interesting adventure.
The most difficult procedure is for children under 3 years of age, as they are very mobile. Before starting the diagnosis, you need to calm the baby down, sit him on your lap, and read a fairy tale.
It’s not easy with hyperactive children either. Hysteria or screaming can distort the results of the examination. The child needs to be distracted so that the doctor has time to record the necessary indicators.
Routine method
This is the standard way to conduct an EEG and is usually prescribed by a pediatrician or neurologist after an initial examination. Thanks to this test, doctors can make a diagnosis. The procedure lasts no more than 15 minutes. It consists of the following samples:
- photostimulation - the eye is exposed to flashing electrodes;
- hyperventilation - the baby must take deep breaths and exhale several times;
- audio stimulation - turn on loud sound;
- Monotonous turning on and off of lights.
EEG of sleep for a child
Nighttime sleep monitoring is carried out for epilepsy and is considered one of the most informative methods (especially to track epileptic activity on the EEG). The essence of diagnostics is to fix several phases, namely:
- the period of wakefulness that will last before falling asleep;
- naps;
- night sleep;
- awakening.
The EEG sleep procedure performed on a child is accompanied by a video recording. A study of daytime and nighttime sleep is also carried out.
With sleep deprivation
When routine electroencephalography does not provide the necessary information, a deprivation study is prescribed, that is, deprivation of night sleep completely or partially. To carry out such a procedure, the patient is either not allowed to sleep at all, or is woken up a couple of hours before waking up, it depends on age:
- preschoolers - rest for 4-6 hours;
- patients 7-11 years old - go to bed at night between 18:00 and 20:00, they are woken up at midnight, EEG is performed at 8-9 am;
- patients over 12 – staying awake for 18 hours or more is practiced.
Decoding of electroencephalogram indicators
In order to decipher the EEG and not miss any of the smallest manifestations in the recording, the specialist needs to take into account all the important points that may affect the indicators being studied. These include age, the presence of certain diseases, possible contraindications and other factors.
Upon completion of the collection of all data from the procedure and their processing, the analysis is completed and then a final conclusion is formed, which will be provided for making a further decision on the choice of therapy method. Any disturbance in activity may be a symptom of diseases caused by certain factors.
Alpha rhythm
The normal frequency is determined in the range of 8–13 Hz, and its amplitude does not go beyond 100 μV. Such characteristics indicate a healthy state of a person and the absence of any pathologies. The following are considered violations:
- constant fixation of the alpha rhythm in the frontal lobe;
- exceeding the difference between the hemispheres by up to 35%;
- constant violation of wave sinusoidality;
- presence of frequency dispersion;
- amplitude below 25 μV and above 95 μV.
The presence of disturbances in this indicator indicates a possible asymmetry of the hemispheres, which may be the result of oncological tumors or pathologies of cerebral circulation, for example, stroke or hemorrhage. A high frequency indicates brain damage or TBI (traumatic brain injury).
Stroke or hemorrhage is one of the possible diagnoses for functional changes in the alpha rhythm
A complete absence of the alpha rhythm is often observed in dementia, and in children, deviations from the norm are directly related to mental retardation (MDD). Such a delay in children is evidenced by: disorganization of alpha waves, shift of focus from the occipital region, increased synchrony, short activation reaction, overreaction to intense breathing.
These manifestations can be caused by inhibitory psychopathy, epileptic seizures, and a short reaction is considered one of the primary signs of neurotic disorders.
Beta rhythm
In the accepted norm, these waves are clearly detected in the frontal lobes of the brain with a symmetrical amplitude in the range of 3–5 μV, recorded in both hemispheres. A high amplitude leads doctors to think about the presence of a concussion, and when short spindles appear, to the occurrence of encephalitis. An increase in the frequency and duration of spindles indicates the development of inflammation.
In children, the pathological manifestations of beta oscillations are considered to be a frequency of 15-16 Hz and a high amplitude present - 40-50 µV, and if its localization is the central or anterior part of the brain, then this should alert the doctor. Such characteristics indicate a high probability of delayed development of the baby.
Delta and theta rhythms
An increase in the amplitude of these indicators above 45 μV on a constant basis is characteristic of functional brain disorders. If the indicators are increased in all brain regions, then this may indicate severe dysfunction of the central nervous system.
If a high amplitude of the delta rhythm is detected, a tumor is suspected. Inflated values of the theta and delta rhythm recorded in the occipital region indicate a child’s lethargy and a delay in his development, as well as impaired circulatory function.
How to get correct results?
EEG of the brain in children of preschool and primary school age is most often carried out in the presence of parents (babies are held in their arms). No special training is required; parents should follow a few simple recommendations:
- Carefully examine the child's head. If there are minor scratches, wounds, scratches, inform your doctor. Electrodes are not attached to areas with damaged epidermis (skin).
- Feed the child. The study is carried out on a full stomach, so as not to blur the indicators. (Sweets containing chocolate, which excites the nervous system, should be excluded from the menu). As for infants, they must be fed immediately before the procedure in a medical facility. In this case, the baby will fall asleep peacefully and the study will be carried out during sleep.
It is more convenient for infants to conduct research during natural sleep
It is important to stop taking medications (if the baby is receiving treatment on an ongoing basis, you need to notify the doctor about this). Children of school and preschool age need to be explained what they have to do and why. The right psychological attitude will help you avoid excessive emotionality. You are allowed to take toys with you (excluding digital gadgets).
You should remove hairpins and bows from your head, and remove earrings from your ears. Girls should not wear their hair in braids. If the EEG is repeated, it is necessary to take the protocol of the previous study. Before the examination, the child's hair and scalp should be washed. One of the conditions is the good health of the little patient. If the child has a cold or other health problems, it is better to postpone the procedure until complete recovery.
Decoding values in different age intervals
An EEG recording of a premature baby at 25–28 gestational weeks looks like a curve in the form of slow flashes of delta and theta rhythms, periodically combined with sharp wave peaks 3–15 seconds long with a decrease in amplitude to 25 μV. In full-term infants, these values are clearly divided into three types of indicators. During wakefulness (with a periodic frequency of 5 Hz and an amplitude of 55–60 Hz), the active phase of sleep (with a stable frequency of 5–7 Hz and a fast low amplitude) and quiet sleep with flashes of delta oscillations at a high amplitude.
Over the course of 3-6 months of a child’s life, the number of theta oscillations is constantly growing, while the delta rhythm, on the contrary, is characterized by a decline. Further, from 7 months to a year, the child develops alpha waves, and delta and theta gradually fade away. Over the next 8 years, the EEG shows a gradual replacement of slow waves with fast ones - alpha and beta oscillations.
Rhythm indicators undergo regular changes depending on age
Until the age of 15, alpha waves predominate, and by the age of 18, the BEA transformation is complete. Over the period from 21 to 50 years, stable indicators remain almost unchanged. And from 50, the next phase of rhythmicity restructuring begins, which is characterized by a decrease in the amplitude of alpha oscillations and an increase in beta and delta.
After 60 years, the frequency also begins to gradually fade, and in a healthy person, manifestations of delta and theta oscillations are noticed on the EEG. According to statistics, age indicators from 1 to 21 years, considered “healthy,” are determined in subjects 1–15 years old, reaching 70%, and in the range of 16–21 – about 80%.
Preparation for analysis and algorithm
To prepare for an electroencephalogram, no special manipulations are required. The main thing is to tell the patient in detail about the procedure and the algorithm for its implementation. This is especially important when conducting an EEG on a child. Since a large number of wires can frighten him, it is necessary to clearly explain that this procedure is absolutely safe and painless.
During the EEG, the person must be calm and relaxed.
Recording of electroencephalogram rhythms is carried out in a sitting or lying position, with eyes closed. The device itself is a cap with electrodes on it, which are lubricated with a contact agent and connected to the recording part of the device.
In this case, pulses captured by the electrodes and a video recording of the patient are simultaneously recorded. In this way, it is possible to compare a convulsive attack and changes in EEG rhythms. With the help of video monitoring, it becomes possible to differentiate a real seizure from a simulation. So, if the video shows a change in the patient's behavior, but the EEG shows the same activity as before, this means that the person is malingering. But there are also options when seizures are not associated with changes in brain activity, for example, with hysterical neuroses.
The most common diagnosed pathologies
Thanks to the electroencephalogram, diseases such as epilepsy or various types of traumatic brain injury (TBI) are quite easily diagnosed.
Epilepsy
The study allows you to determine the localization of the pathological area, as well as the specific type of epileptic disease. At the time of a convulsive syndrome, the EEG recording has a number of specific manifestations:
- pointed waves (peaks) - suddenly rising and falling can appear in one or several areas;
- the combination of slow pointed waves during an attack becomes even more pronounced;
- sudden increase in amplitude in the form of flashes.
The use of stimulating artificial signals helps in determining the form of epileptic disease, since they provide visibility of hidden activity that is difficult to diagnose with EEG. For example, intense breathing, requiring hyperventilation, leads to a decrease in the lumen of blood vessels.
Photostimulation is also used, carried out using a strobe (a powerful light source), and if there is no reaction to the stimulus, then most likely there is a pathology associated with the conduction of visual impulses. The appearance of non-standard vibrations indicates pathological changes in the brain. The doctor should not forget that exposure to powerful light can lead to an epileptic seizure.
Who needs an EEG and when?
Electroencephalography provides the most complete picture of the state of the central nervous system. Therefore, diagnosis using EEG has a wide range of applications.
So, it is prescribed for:
- Assessment of brain maturity and functionality in a premature infant or an infant born as a result of a pathological pregnancy.
- Determining the causes of sleep disorders (insomnia, excessive sleepiness, etc.).
- Finding the cause of convulsive conditions and epileptic seizures.
- Confirmation (refutation) of the presence of complications of inflammatory processes resulting from neuroinfection.
- Assess the effects of exposure to neurotoxins.
Such a study is of particular importance in the following cases:
- Vascular disorders in the brain.
- Traumatic brain injuries (head concussion or concussion). EEG allows you to identify the degree of disturbances and determine how to eliminate them.
- Suspicion of the development of a tumor affecting the central nervous system.
- Development of various mental disorders.
- When an assessment of the effectiveness of anticonvulsant therapy is required.
- When selecting medications and their dosage for the treatment of epileptic seizures.
- When there are suspicions of pathological changes in the brain in elderly patients (Parkinson's disease, Alzheimer's disease, etc.).
Important. An EEG is necessary if it is impossible to use other diagnostic methods, for example, if the patient is in a coma.
In addition, studies of brain activity require:
- Surgical intervention (the effect of anesthesia and its depth are determined).
- Various forms of disorders of different parts of the central nervous system.
- Comatose states (to establish the death of more brain cells), and many other situations.
EEG is prescribed to conscripts prone to manifestations of convulsive syndrome or loss of consciousness, as well as to vehicle drivers.
Tags: EEG
Discussion: there is 1 comment
- Moroshkin Vladimir Vasilievich:
05/11/2019 at 07:39Thank you thank you thank you!